- Diabetes, obesity and metabolism
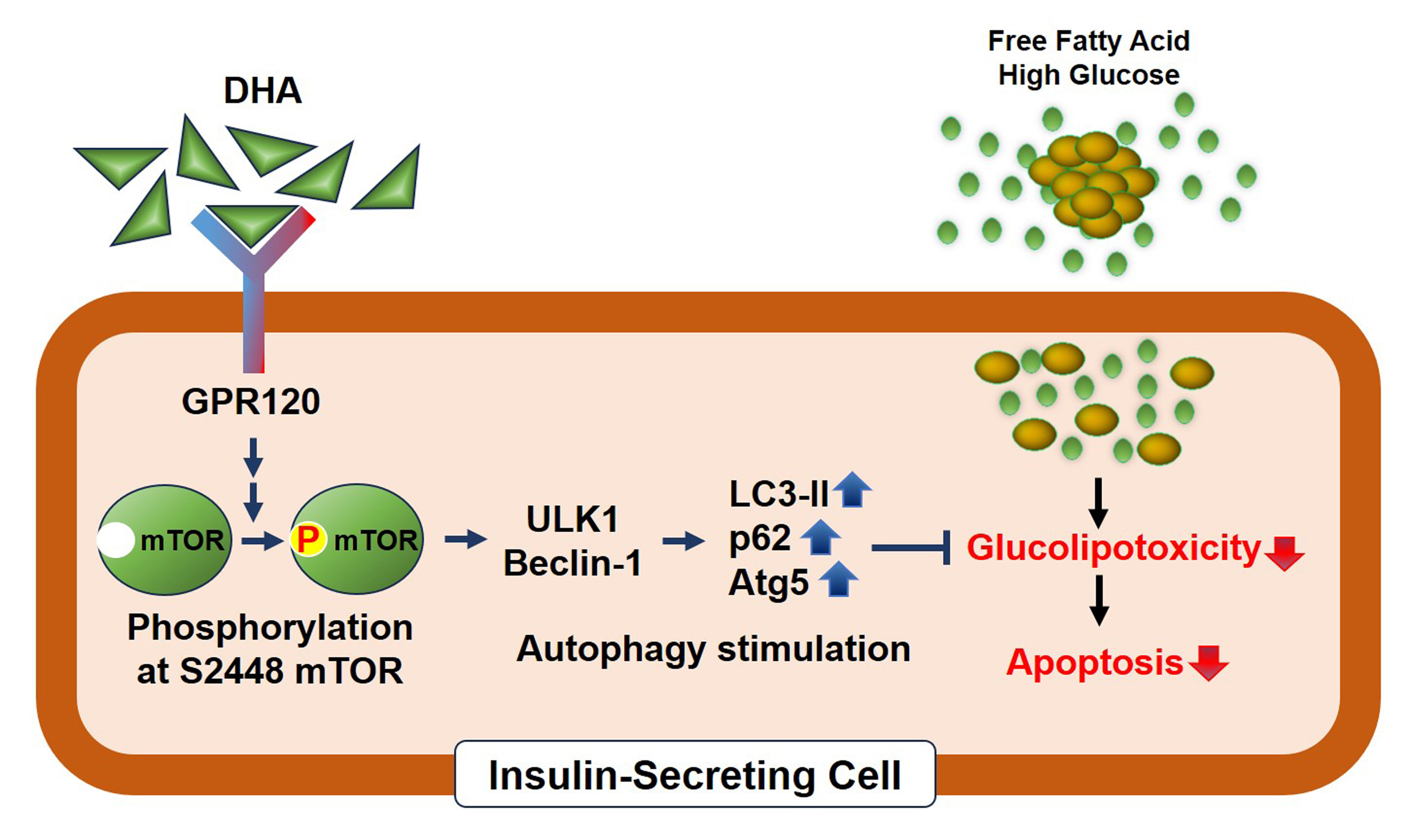
- Docosahexanoic Acid Attenuates Palmitate-Induced Apoptosis by Autophagy Upregulation via GPR120/mTOR Axis in Insulin-Secreting Cells
-
Seok-Woo Hong, Jinmi Lee, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2024;39(2):353-363. Published online January 23, 2024
-
DOI: https://doi.org/10.3803/EnM.2023.1809
-
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Polyunsaturated fatty acids (PUFAs) reportedly have protective effects on pancreatic β-cells; however, the underlying mechanisms are unknown.
Methods
To investigate the cellular mechanism of PUFA-induced cell protection, mouse insulinoma 6 (MIN6) cells were cultured with palmitic acid (PA) and/or docosahexaenoic acid (DHA), and alterations in cellular signaling and apoptosis were examined.
Results
DHA treatment remarkably repressed caspase-3 cleavage and terminal deoxynucleotidyl transferase-mediated UTP nick end labeling (TUNEL)-positive red dot signals in PA-treated MIN6 cells, with upregulation of autophagy, an increase in microtubule- associated protein 1-light chain 3 (LC3)-II, autophagy-related 5 (Atg5), and decreased p62. Upstream factors involved in autophagy regulation (Beclin-1, unc51 like autophagy activating kinase 1 [ULK1], phosphorylated mammalian target of rapamycin [mTOR], and protein kinase B) were also altered by DHA treatment. DHA specifically induced phosphorylation on S2448 in mTOR; however, phosphorylation on S2481 decreased. The role of G protein-coupled receptor 120 (GPR120) in the effect of DHA was demonstrated using a GPR120 agonist and antagonist. Additional treatment with AH7614, a GPR120 antagonist, significantly attenuated DHA-induced autophagy and protection. Taken together, DHA-induced autophagy activation with protection against PA-induced apoptosis mediated by the GPR120/mTOR axis.
Conclusion
These findings indicate that DHA has therapeutic effects on PA-induced pancreatic β-cells, and that the cellular mechanism of β-cell protection by DHA may be a new research target with potential pharmacotherapeutic implications in β-cell protection.
- Diabetes, obesity and metabolism
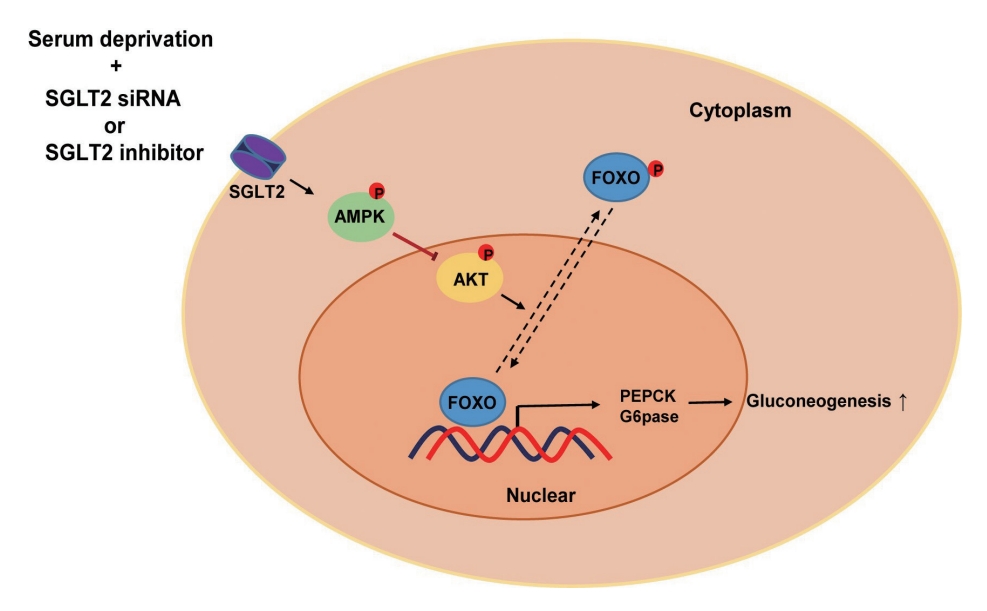
- Inhibition of Sodium-Glucose Cotransporter-2 during Serum Deprivation Increases Hepatic Gluconeogenesis via the AMPK/AKT/FOXO Signaling Pathway
-
Jinmi Lee, Seok-Woo Hong, Min-Jeong Kim, Yu-Mi Lim, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2024;39(1):98-108. Published online January 3, 2024
-
DOI: https://doi.org/10.3803/EnM.2023.1786
-
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Sodium-dependent glucose cotransporter 2 (SGLT2) mediates glucose reabsorption in the renal proximal tubules, and SGLT2 inhibitors are used as therapeutic agents for treating type 2 diabetes mellitus. This study aimed to elucidate the effects and mechanisms of SGLT2 inhibition on hepatic glucose metabolism in both serum deprivation and serum supplementation states.
Methods
Huh7 cells were treated with the SGLT2 inhibitors empagliflozin and dapagliflozin to examine the effect of SGLT2 on hepatic glucose uptake. To examine the modulation of glucose metabolism by SGLT2 inhibition under serum deprivation and serum supplementation conditions, HepG2 cells were transfected with SGLT2 small interfering RNA (siRNA), cultured in serum-free Dulbecco’s modified Eagle’s medium for 16 hours, and then cultured in media supplemented with or without 10% fetal bovine serum for 8 hours.
Results
SGLT2 inhibitors dose-dependently decreased hepatic glucose uptake. Serum deprivation increased the expression levels of the gluconeogenesis genes peroxisome proliferator-activated receptor gamma co-activator 1 alpha (PGC-1α), glucose 6-phosphatase (G6pase), and phosphoenolpyruvate carboxykinase (PEPCK), and their expression levels during serum deprivation were further increased in cells transfected with SGLT2 siRNA. SGLT2 inhibition by siRNA during serum deprivation induces nuclear localization of the transcription factor forkhead box class O 1 (FOXO1), decreases nuclear phosphorylated-AKT (p-AKT), and p-FOXO1 protein expression, and increases phosphorylated-adenosine monophosphate-activated protein kinase (p-AMPK) protein expression. However, treatment with the AMPK inhibitor, compound C, reversed the reduction in the protein expression levels of nuclear p- AKT and p-FOXO1 and decreased the protein expression levels of p-AMPK and PEPCK in cells transfected with SGLT2 siRNA during serum deprivation.
Conclusion
These data show that SGLT2 mediates glucose uptake in hepatocytes and that SGLT2 inhibition during serum deprivation increases gluconeogenesis via the AMPK/AKT/FOXO1 signaling pathway.
- Diabetes, obesity and metabolism
- Coronary Artery Calcium Score as a Sensitive Indicator of Cardiovascular Disease in Patients with Type 2 Diabetes Mellitus: A Long-Term Cohort Study
-
Dae-Jeong Koo, Mi Yeon Lee, Sun Joon Moon, Hyemi Kwon, Sang Min Lee, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki Won Oh, Sung Rae Cho, Young-Hoon Jeong, Eun-Jung Rhee
-
Endocrinol Metab. 2023;38(5):568-577. Published online October 10, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1770
-
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Coronary artery calcium score (CACS) has become an important tool for evaluating cardiovascular disease (CVD). This study evaluated the significance of CACS for future CVD through more than 10 years of follow-up in asymptomatic Korean populations with type 2 diabetes mellitus (T2DM) known to have a relatively low CACS burden.
Methods
We enrolled 981 asymptomatic T2DM patients without CVD at baseline who underwent CACS evaluation using multidetector computed tomography between January 2008 and December 2014. They were grouped into five predefined CACS categories based on Agatston scores and followed up by August 2020. The primary endpoint was incident CVD events, including coronary, cerebrovascular, and peripheral arterial disease.
Results
The relative risk of CVD was significantly higher in patients with CACS ≥10, and the significance persisted after adjustment for known confounders. A higher CACS category indicated a higher incidence of future CVD: hazard ratio (95% confidence interval) 4.09 (1.79 to 9.36), 12.00 (5.61 to 25.69), and 38.79 (16.43 to 91.59) for 10≤ CACS <100, 100≤ CACS <400, and CACS ≥400, respectively. During the 12-year follow-up period, the difference in event-free survival more than doubled as the category increased. Patients with CACS below 10 had very low CVD incidence throughout the follow-up. The receiver operating characteristic analysis showed better area under curve when the CACS cutoff was 10 than 100.
Conclusion
CACS can be a sensitive marker of CVD risk. Specifically, CACS above 10 is an indicator of CVD high-risk requiring more intensive medical treatment in Koreans with T2DM.
- Thyroid
- The Current Status of Hyperthyroidism in Korea
-
Hyemi Kwon
-
Endocrinol Metab. 2023;38(4):392-394. Published online August 25, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.401
-
-
 PDF PDF PubReader PubReader  ePub ePub
- Miscellaneous
- Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
-
Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim, The Committee of Clinical Practice Guideline of the Korean Endocrine Society
-
Endocrinol Metab. 2022;37(6):839-850. Published online December 26, 2022
-
DOI: https://doi.org/10.3803/EnM.2022.1627
-
-
3,553
View
-
321
Download
-
2
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
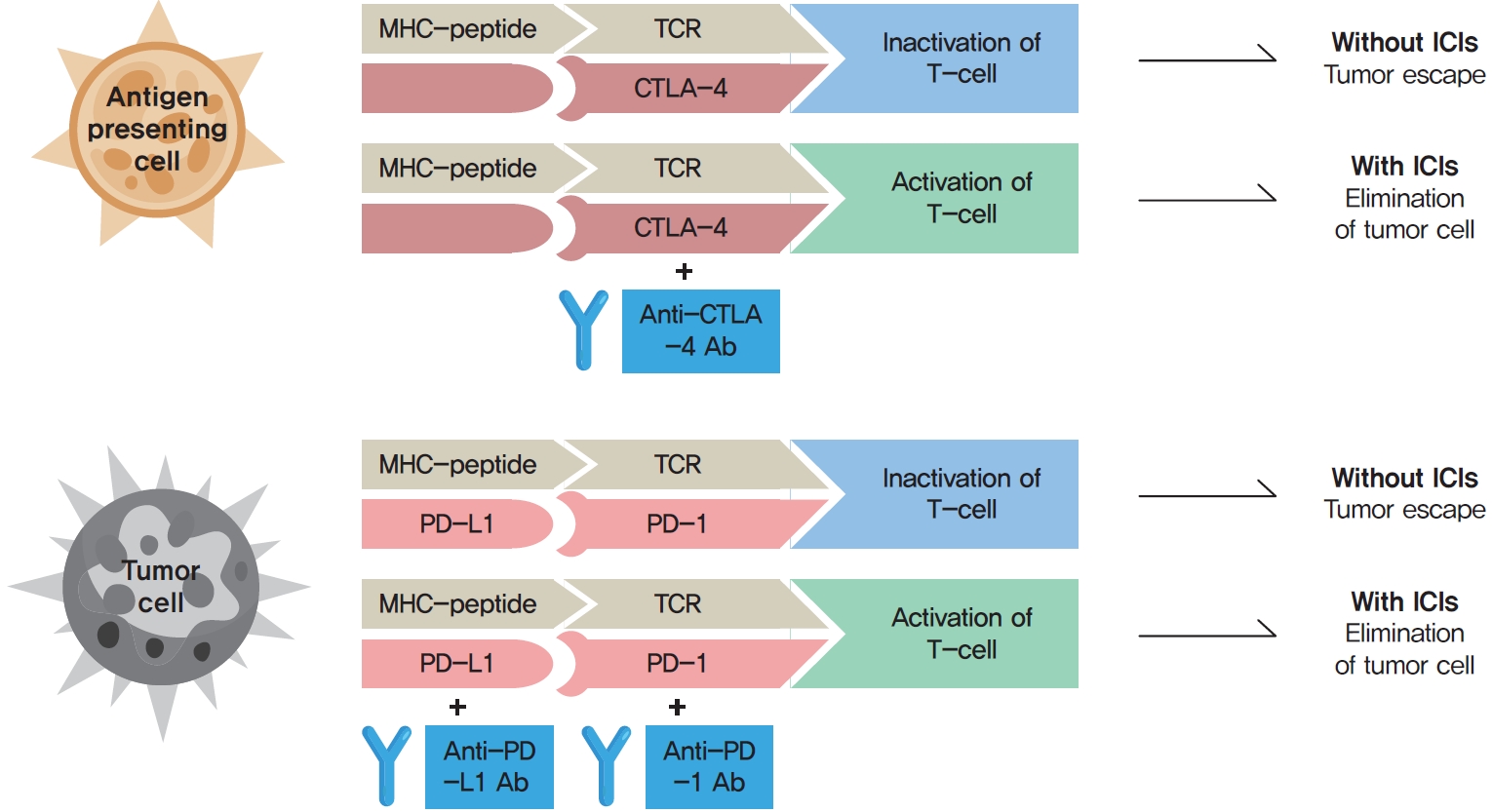
- Immune checkpoint inhibitors (ICIs) including an anti-cytotoxic T-lymphocyte-associated antigen 4 inhibitor, anti-programmed cell death protein 1 (PD-1) inhibitors, and anti-PD-ligand 1 inhibitors are representative therapeutics for various malignancies. In oncology, the application of ICIs is currently expanding to a wider range of malignancies due to their remarkable clinical outcomes. ICIs target immune checkpoints which suppress the activity of T-cells that are specific for tumor antigens, thereby allowing tumor cells to escape the immune response. However, immune checkpoints also play a crucial role in preventing autoimmune reactions. Therefore, ICIs targeting immune checkpoints can trigger various immune-related adverse events (irAEs), especially in endocrine organs. Considering the endocrine organs that are frequently involved, irAEs associated endocrinopathies are frequently life-threatening and have unfavorable clinical implications for patients. However, there are very limited data from large clinical trials that would inform the development of clinical guidelines for patients with irAEs associated endocrinopathies. Considering the current clinical situation, in which the scope and scale of the application of ICIs are increasing, position statements from clinical specialists play an essential role in providing the appropriate recommendations based on both medical evidence and clinical experience. As endocrinologists, we would like to present precautions and recommendations for the management of immune-related endocrine disorders, especially those involving the adrenal, thyroid, and pituitary glands caused by ICIs.
-
Citations
Citations to this article as recorded by  - Pembrolizumab plus lenvatinib for radically unresectable or metastatic renal cell carcinoma in the Japanese population
Ryo Fujiwara, Takeshi yuasa, kenichi kobayashi, tetsuya yoshida, susumu kageyama
Expert Review of Anticancer Therapy.2023; 23(5): 461. CrossRef - Incidence of Endocrine-Related Dysfunction in Patients Treated with New Immune Checkpoint Inhibitors: A Meta-Analysis and Comprehensive Review
Won Sang Yoo, Eu Jeong Ku, Eun Kyung Lee, Hwa Young Ahn
Endocrinology and Metabolism.2023; 38(6): 750. CrossRef
- Diabetes, Obesity and Metabolism
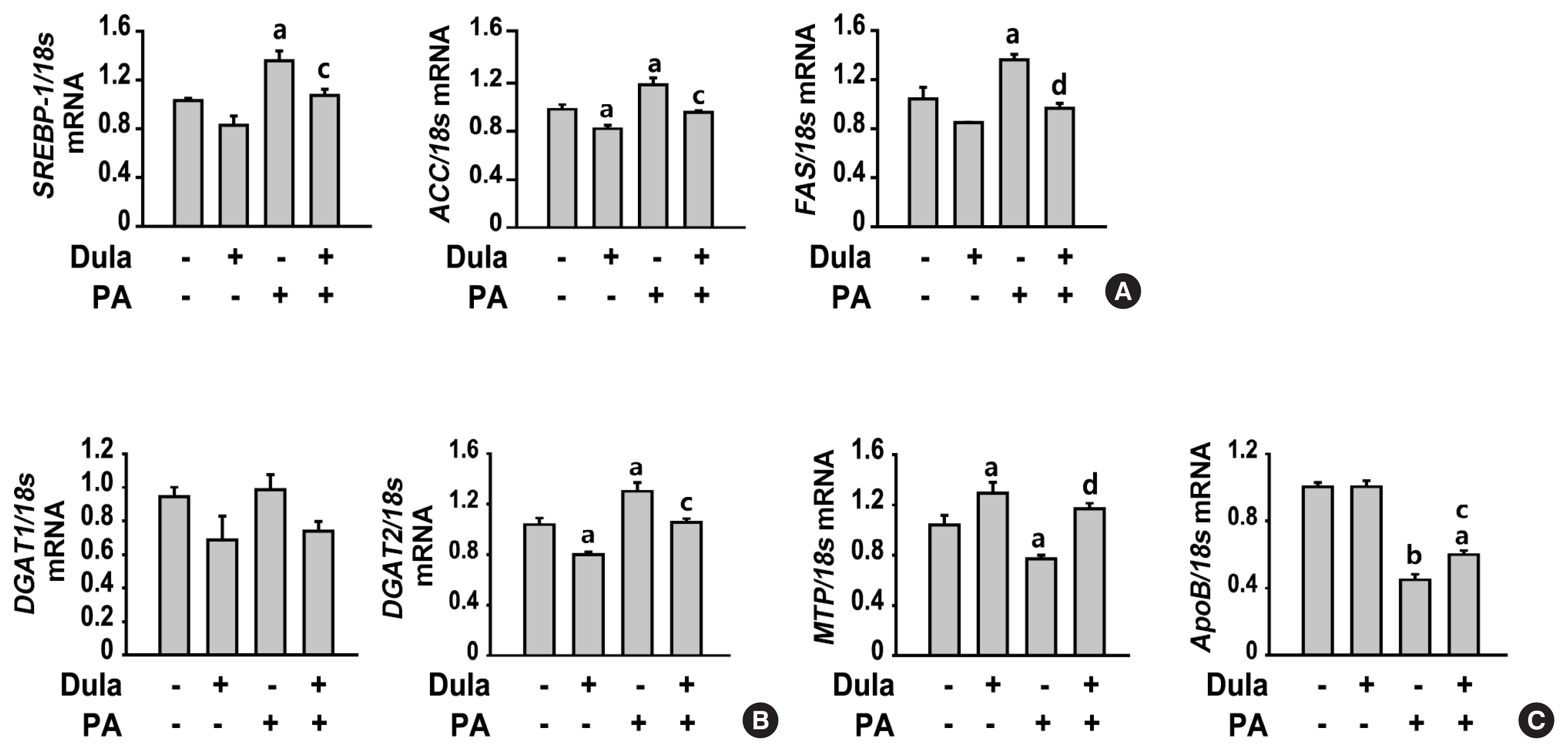
- Dulaglutide Ameliorates Palmitic Acid-Induced Hepatic Steatosis by Activating FAM3A Signaling Pathway
-
Jinmi Lee, Seok-Woo Hong, Min-Jeong Kim, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2022;37(1):74-83. Published online February 9, 2022
-
DOI: https://doi.org/10.3803/EnM.2021.1293
-
-
4,937
View
-
235
Download
-
5
Web of Science
-
5
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Dulaglutide, a long-acting glucagon-like peptide-1 receptor agonist (GLP-1RA), has been shown to reduce body weight and liver fat content in patients with type 2 diabetes. Family with sequence similarity 3 member A (FAM3A) plays a vital role in regulating glucose and lipid metabolism. The aim of this study was to determine the mechanisms by which dulaglutide protects against hepatic steatosis in HepG2 cells treated with palmitic acid (PA).
Methods
HepG2 cells were pretreated with 400 μM PA for 24 hours, followed by treatment with or without 100 nM dulaglutide for 24 hours. Hepatic lipid accumulation was determined using Oil red O staining and triglyceride (TG) assay, and the expression of lipid metabolism-associated factor was analyzed using quantitative real time polymerase chain reaction and Western blotting.
Results
Dulaglutide significantly decreased hepatic lipid accumulation and reduced the expression of genes associated with lipid droplet binding proteins, de novo lipogenesis, and TG synthesis in PA-treated HepG2 cells. Dulaglutide also increased the expression of proteins associated with lipolysis and fatty acid oxidation and FAM3A in PA-treated cells. However, exendin-(9-39), a GLP-1R antagonist, reversed the expression of FAM3A, and fatty acid oxidation-associated factors increased due to dulaglutide. In addition, inhibition of FAM3A by siRNA attenuated the reducing effect of dulaglutide on TG content and its increasing effect on regulation of fatty acid oxidation.
Conclusion
These results suggest that dulaglutide could be used therapeutically for improving nonalcoholic fatty liver disease, and its effect could be mediated in part via upregulation of FAM3A expression through a GLP-1R-dependent pathway.
-
Citations
Citations to this article as recorded by  - GLP-1/GLP-1RAs: New Options for the Drug Treatment of NAFLD
Haoran Jiang, Linquan Zang
Current Pharmaceutical Design.2024; 30(2): 100. CrossRef - GLP-1 Receptor Agonists in Non-Alcoholic Fatty Liver Disease: Current Evidence and Future Perspectives
Riccardo Nevola, Raffaella Epifani, Simona Imbriani, Giovanni Tortorella, Concetta Aprea, Raffaele Galiero, Luca Rinaldi, Raffaele Marfella, Ferdinando Carlo Sasso
International Journal of Molecular Sciences.2023; 24(2): 1703. CrossRef - FAM3A mediates the phenotypic switch of human aortic smooth muscle cells stimulated with oxidised low-density lipoprotein by influencing the PI3K-AKT pathway
Lei Yang, Baoshun Du, Shitao Zhang, Maode Wang
In Vitro Cellular & Developmental Biology - Animal.2023; 59(6): 431. CrossRef - ATP Secretion and Metabolism in Regulating Pancreatic Beta Cell Functions and Hepatic Glycolipid Metabolism
Jing Li, Han Yan, Rui Xiang, Weili Yang, Jingjing Ye, Ruili Yin, Jichun Yang, Yujing Chi
Frontiers in Physiology.2022;[Epub] CrossRef - Targeted therapeutics and novel signaling pathways in non-alcohol-associated fatty liver/steatohepatitis (NAFL/NASH)
Xiaohan Xu, Kyle L. Poulsen, Lijuan Wu, Shan Liu, Tatsunori Miyata, Qiaoling Song, Qingda Wei, Chenyang Zhao, Chunhua Lin, Jinbo Yang
Signal Transduction and Targeted Therapy.2022;[Epub] CrossRef
- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database)
- The Effects of Glucose Lowering Agents on the Secondary Prevention of Coronary Artery Disease in Patients with Type 2 Diabetes
-
Inha Jung, Hyemi Kwon, Se Eun Park, Kyung-Do Han, Yong-Gyu Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2021;36(5):977-987. Published online October 14, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.1046
-
-
4,055
View
-
175
Download
-
3
Web of Science
-
3
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Patients with diabetes have a higher risk of requiring repeated percutaneous coronary intervention (PCI) than non-diabetic patients. We aimed to evaluate and compare the effects of anti-diabetic drugs on the secondary prevention of myocardial infarction among type 2 diabetes mellitus patients.
Methods
We analyzed the general health check-up dataset and claims data of the Korean National Health Insurance Service of 199,714 participants (age ≥30 years) who underwent PCIs between 2010 and 2013. Those who underwent additional PCI within 1 year of their first PCI (n=3,325) and those who died within 1 year (n=1,312) were excluded. Patients were classified according to their prescription records for glucose-lowering agents. The primary endpoint was the incidence rate of coronary revascularization.
Results
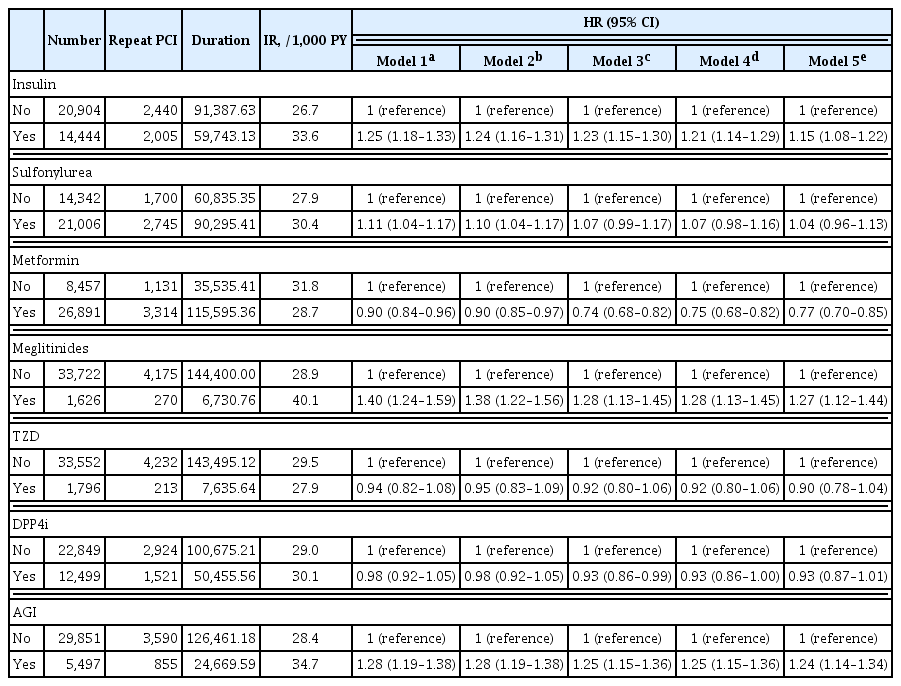
A total of 35,348 patients were included in the study. Metformin significantly decreased the risk of requiring repeat PCI in all patients (adjusted hazard ratio [aHR], 0.77). In obese patients with body mass index (BMI) ≥25 kg/m2, patients treated with thiazolidinedione (TZD) exhibited a decreased risk of requiring repeat revascularization than those who were not treated with TZD (aHR, 0.77; 95% confidence interval, 0.63 to 0.95). Patients treated with metformin showed a decreased risk of requiring revascularization regardless of their BMI. Insulin, meglitinide, and alpha-glucosidase inhibitor were associated with increased risk of repeated PCI.
Conclusion
The risk of requiring repeat revascularization was lower in diabetic patients treated with metformin and in obese patients treated with TZD. These results suggest that physicians should choose appropriate glucose-lowering agents for the secondary prevention of coronary artery disease.
-
Citations
Citations to this article as recorded by  - Application of systemic inflammation indices and lipid metabolism-related factors in coronary artery disease
Zhuoyan Zhao, Huan Lian, Yixiang Liu, Lixian Sun, Ying Zhang
Coronary Artery Disease.2023; 34(5): 306. CrossRef - Effect of metformin on adverse outcomes in T2DM patients: Systemic review and meta-analysis of observational studies
Zhicheng Xu, Haidong Zhang, Chenghui Wu, Yuxiang Zheng, Jingzhou Jiang
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Establishment of a Predictive Model for Poor Prognosis of Incomplete Revascularization in Patients with Coronary Heart Disease and Multivessel Disease
Huan Lian, Zhuoyan Zhao, Kelin Ma, Zhenjiang Ding, Lixian Sun, Ying Zhang
Clinical and Applied Thrombosis/Hemostasis.2022; 28: 107602962211392. CrossRef
- Diabetes, Obesity and Metabolism
- Changes in Insulin Resistance Index and the Risk of Liver Fibrosis in Patients with Nonalcoholic Fatty Liver Disease without Diabetes: Kangbuk Samsung Health Study
-
Dae-Jeong Koo, Mi Yeon Lee, Inha Jung, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2021;36(5):1016-1028. Published online October 21, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.1110
-
-
4,196
View
-
129
Download
-
5
Web of Science
-
7
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Fibrosis is the most important prognostic factor for nonalcoholic fatty liver disease (NAFLD). Insulin resistance plays a key role of fibrosis progression. We evaluated the association between changes in homeostasis model assessment of insulin resistance (HOMA-IR) values and changes in fibrosis status in NAFLD.
Methods
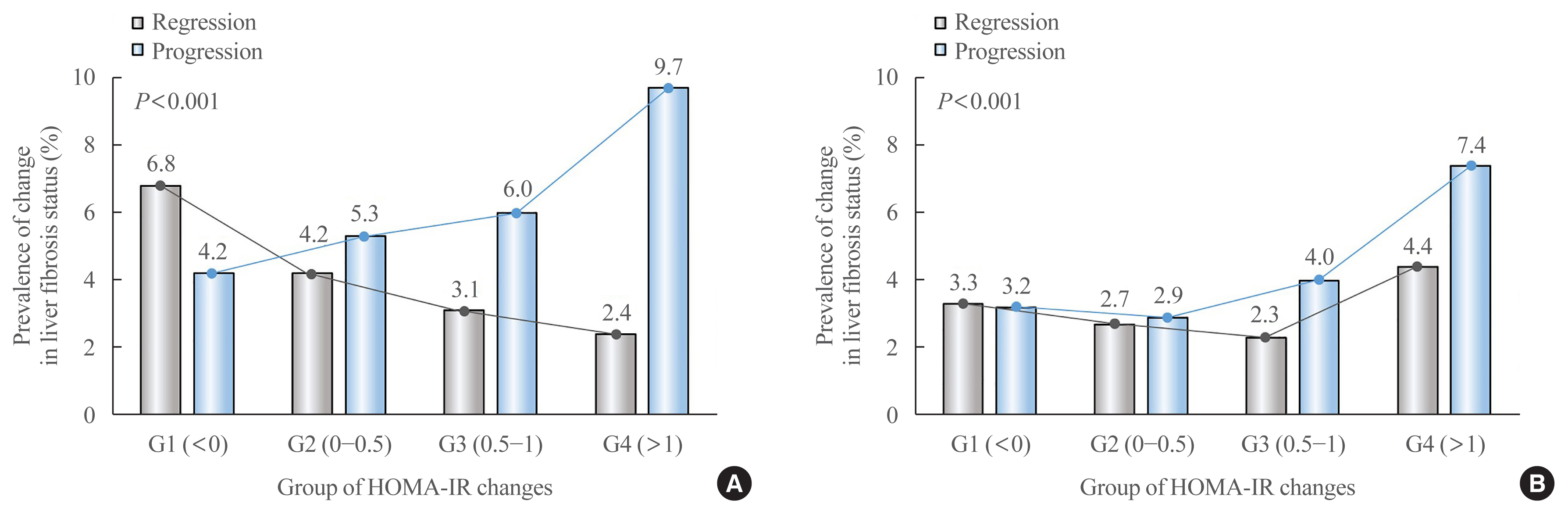
We analyzed the data of 15,728 participants with NAFLD (86% men, mean age 40.5 years) who had no diabetes at baseline and visited our centers for health check-ups both in 2012 and 2016. The participants were classified into four groups according to the degree of change in HOMA-IR values from baseline to the end of follow-up: G1 (<0), G2 (0–0.50), G3 (0.51–1.00), and G4 (>1.00). NAFLD was assessed by ultrasonography, and fibrosis status was evaluated by the NAFLD fibrosis score (NFS) and the aspartate aminotransferase to platelet ratio index (APRI).
Results
After the 4-year follow-up, the multivariable-adjusted odds ratio (OR) for progression of fibrosis probability increased with increasing HOMA-IR values (OR, 2.25; 95% confidence interval [CI], 1.87 to 2.71 for NFS; and OR, 2.55; 95% CI, 2.05 to 3.18 for APRI, G4). This tendency remained consistent throughout the subgroup analyses, except in those for female sex and a body mass index <25 kg/m2. The OR for regression of fibrosis probability decreased with increasing HOMA-IR values (OR, 0.33; 95% CI, 0.25 to 0.43 for NFS, G4).
Conclusion
Changes in HOMA-IR values were associated with changes in fibrosis status in patients with NAFLD without diabetes, which underscores the role of insulin resistance in liver fibrosis.
-
Citations
Citations to this article as recorded by  - Insulin Resistance/Sensitivity Measures as Screening Indicators of Metabolic-Associated Fatty Liver Disease and Liver Fibrosis
Mohammad E. Khamseh, Mojtaba Malek, Soodeh Jahangiri, Sohrab Nobarani, Azita Hekmatdoost, Marieh Salavatizadeh, Samira Soltanieh, Haleh Chehrehgosha, Hoda Taheri, Zeinab Montazeri, Fereshteh Attaran, Faramarz Ismail-Beigi, Fariba Alaei-Shahmiri
Digestive Diseases and Sciences.2024; 69(4): 1430. CrossRef - Association between nonalcoholic fatty liver disease and left ventricular diastolic dysfunction: A 7-year retrospective cohort study of 3,380 adults using serial echocardiography
Gyuri Kim, Tae Yang Yu, Jae Hwan Jee, Ji Cheol Bae, Mira Kang, Jae Hyeon Kim
Diabetes & Metabolism.2024; 50(3): 101534. CrossRef - Factors Associated with Liver Fibrosis in Chinese Patients with Type 2 Diabetes Mellitus and Non-Alcoholic Fatty Liver Disease
Yu Luo, Cuiyu Wang, Tian Zhang, Xiaoyu He, Jianan Hao, Andong Shen, Hang Zhao, Shuchun Chen, Luping Ren
International Journal of General Medicine.2023; Volume 16: 293. CrossRef - Impact of COVID-19 Lockdown on Non-Alcoholic Fatty Liver Disease and Insulin Resistance in Adults: A before and after Pandemic Lockdown Longitudinal Study
Ángel Arturo López-González, Bárbara Altisench Jané, Luis Masmiquel Comas, Sebastiana Arroyo Bote, Hilda María González San Miguel, José Ignacio Ramírez Manent
Nutrients.2022; 14(14): 2795. CrossRef - Metabolic Score for Insulin Resistance Is Inversely Related to Incident Advanced Liver Fibrosis in Patients with Non-Alcoholic Fatty Liver Disease
Jun-Hyuk Lee, Yu-Jin Kwon, Kyongmin Park, Hye Sun Lee, Hoon-Ki Park, Jee Hye Han, Sang Bong Ahn
Nutrients.2022; 14(15): 3039. CrossRef - Machine learning models including insulin resistance indexes for predicting liver stiffness in United States population: Data from NHANES
Kexing Han, Kexuan Tan, Jiapei Shen, Yuting Gu, Zilong Wang, Jiayu He, Luyang Kang, Weijie Sun, Long Gao, Yufeng Gao
Frontiers in Public Health.2022;[Epub] CrossRef - The crosstalk between insulin resistance and nonalcoholic fatty liver disease/metabolic dysfunction-associated fatty liver disease: a culprit or a consequence?
Dae-Jeong Koo, Won-Young Lee
Cardiovascular Prevention and Pharmacotherapy.2022; 4(4): 132. CrossRef
- Miscellaneous
- COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
-
Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim, the Committee of Clinical Practice Guideline of the Korean Endocrine Society
-
Endocrinol Metab. 2021;36(4):757-765. Published online August 17, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.404
-
-
10,421
View
-
419
Download
-
19
Web of Science
-
21
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Since the first outbreak of coronavirus disease 2019 (COVID-19), ongoing efforts have been made to discover an efficacious vaccine against COVID-19 to combat the pandemic. In most countries, both mRNA and DNA vaccines have been administered, and their side effects have also been reported. The clinical course of COVID-19 and the effects of vaccination against COVID-19 are both influenced by patients’ health status and involve a systemic physiological response. In view of the systemic function of endocrine hormones, endocrine disorders themselves and the therapeutics used to treat them can influence the outcomes of vaccination for COVID-19. However, there are very limited data to support the development of clinical guidelines for patients with specific medical backgrounds based on large clinical trials. In the current severe circumstances of the COVID-19 pandemic, position statements made by clinical specialists are essential to provide appropriate recommendations based on both medical evidence and clinical experiences. As endocrinologists, we would like to present the medical background of COVID-19 vaccination, as well as precautions to prevent the side effects of COVID-19 vaccination in patients with specific endocrine disorders, including adrenal insufficiency, diabetes mellitus, osteoporosis, autoimmune thyroid disease, hypogonadism, and pituitary disorders.
-
Citations
Citations to this article as recorded by  - COVID-19 mRNA vaccine may trigger subacute thyroiditis
Mehmet Sözen, Ömercan Topaloğlu, Berrin Çetinarslan, Alev Selek, Zeynep Cantürk, Emre Gezer, Damla Köksalan, Taner Bayraktaroğlu
Human Vaccines & Immunotherapeutics.2024; 17(12): 5120. CrossRef - The role of co-morbidities in the development of an AEFI after COVID-19 vaccination in a large prospective cohort with patient-reported outcomes in the Netherlands
C. Ouaddouh, J.W. Duijster, T. Lieber, F.P.A.M. van Hunsel
Expert Opinion on Drug Safety.2024; 23(3): 323. CrossRef - Thyroid dysfunction in COVID-19
David Tak Wai Lui, Chi Ho Lee, Yu Cho Woo, Ivan Fan Ngai Hung, Karen Siu Ling Lam
Nature Reviews Endocrinology.2024;[Epub] CrossRef - Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
Hyeyeon Moon, Sunghwan Suh, Mi Kyoung Park
Journal of Korean Medical Science.2023;[Epub] CrossRef - Prior immunization status of COVID-19 patients and disease severity: A multicenter retrospective cohort study assessing the different types of immunity
Javaria Aslam, Faisal Shahzad Khan, Muhammad Talha Haris, Hewad Hewadmal, Maryam Khalid, Mohammad Y. Alshahrani, Qurrat-ul-ain Aslam, Irrum Aneela, Urooj Zafar
Vaccine.2023; 41(2): 598. CrossRef - Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
Endocrinology and Metabolism.2023; 38(2): 253. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Inactivated SARS-CoV-2 vaccination does not disturb the clinical course of Graves’ disease: An observational cohort study
Shichen Xu, Huixin Yu, Xian Cheng, Jing Wu, Jiandong Bao, Li Zhang
Vaccine.2023; 41(38): 5648. CrossRef - Adrenal Crisis Associated With COVID-19 Vaccination in Patients With Adrenal Insufficiency
Yukako Kurematsu, Takako Mohri, Sadanori Okada, Yutaka Takahashi
JCEM Case Reports.2023;[Epub] CrossRef - Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study
İbrahim Mert Erbaş, İrem Ceren Erbaş, Gözde Akın Kağızmanlı, Kübra Yüksek Acinikli, Özge Besci, Korcan Demir, Ece Böber, Nurşen Belet, Ayhan Abacı
Journal of Clinical Research in Pediatric Endocrinology.2023; 15(3): 248. CrossRef - Neue Aspekte der Glukokortikoidsubstitution bei Nebennierenrindeninsuffizienz
Tina Kienitz, Gesine Meyer
Der Internist.2022; 63(1): 12. CrossRef - Endocrine Follow-up During Post-Acute COVID-19: Practical Recommendations Based on Available Clinical Evidence
Rimesh Pal, Ameya Joshi, Sanjay K. Bhadada, Mainak Banerjee, Suresh Vaikkakara, Satinath Mukhopadhyay
Endocrine Practice.2022; 28(4): 425. CrossRef - Safety of Inactivated and mRNA COVID-19 Vaccination Among Patients Treated for Hypothyroidism: A Population-Based Cohort Study
Xi Xiong, Carlos King Ho Wong, Ivan Chi Ho Au, Francisco Tsz Tsun Lai, Xue Li, Eric Yuk Fai Wan, Celine Sze Ling Chui, Esther Wai Yin Chan, Franco Wing Tak Cheng, Kristy Tsz Kwan Lau, Chi Ho Lee, Yu Cho Woo, David Tak Wai Lui, Ian Chi Kei Wong
Thyroid.2022; 32(5): 505. CrossRef - The New Entity of Subacute Thyroiditis amid the COVID-19 Pandemic: From Infection to Vaccine
Mihaela Popescu, Adina Ghemigian, Corina Maria Vasile, Andrei Costache, Mara Carsote, Alice Elena Ghenea
Diagnostics.2022; 12(4): 960. CrossRef - Adrenal Crisis Secondary to COVID-19 Vaccination in a Patient With Hypopituitarism
Nikolina Markovic, Anila Faizan, Chirag Boradia, Sridhar Nambi
AACE Clinical Case Reports.2022; 8(4): 171. CrossRef - The Effect of Inactivated SARS-CoV-2 Vaccines on TRAB in Graves’ Disease
LingHong Huang, ZhengRong Jiang, JingXiong Zhou, YuPing Chen, HuiBin Huang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Osteoporosis in Patients With Respiratory Diseases
Yue Ma, Shui Qiu, Renyi Zhou
Frontiers in Physiology.2022;[Epub] CrossRef - Pilot Findings on SARS-CoV-2 Vaccine-Induced Pituitary Diseases: A Mini Review from Diagnosis to Pathophysiology
Ach Taieb, El Euch Mounira
Vaccines.2022; 10(12): 2004. CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - No need of glucocorticoid dose adjustment in patients with adrenal insufficiency before COVID-19 vaccine
Tania Pilli, Cristina Dalmiglio, Gilda Dalmazio, Alfonso Sagnella, Raffaella Forleo, Lucia Brilli, Fabio Maino, Cristina Ciuoli, Maria Grazia Castagna
European Journal of Endocrinology.2022; 187(1): K7. CrossRef - Diabetes and COVID-19 Vaccination
Hae Dong Choi, Jun Sung Moon
The Journal of Korean Diabetes.2021; 22(4): 221. CrossRef
- Diabetes, Obesity and Metabolism
- Increased Risk of Nonalcoholic Fatty Liver Disease in Individuals with High Weight Variability
-
Inha Jung, Dae-Jeong Koo, Mi Yeon Lee, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2021;36(4):845-854. Published online August 27, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.1098
-
-
4,968
View
-
140
Download
-
7
Web of Science
-
9
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Weight loss through lifestyle modification is recommended for patients with nonalcoholic fatty liver disease (NAFLD). Recent studies have suggested that repeated loss and gain of weight is associated with worse health outcomes. This study aimed to examine the association between weight variability and the risk of NAFLD in patients without diabetes.
Methods
We examined the health-checkup data of 30,708 participants who had undergone serial examinations between 2010 and 2014. Weight variability was assessed using coefficient of variation and the average successive variability of weight (ASVW), which was defined as the sum of absolute weight changes between successive years over the 5-year period divided by 4. The participants were classified according to the baseline body mass index and weight difference over 4 years.
Results
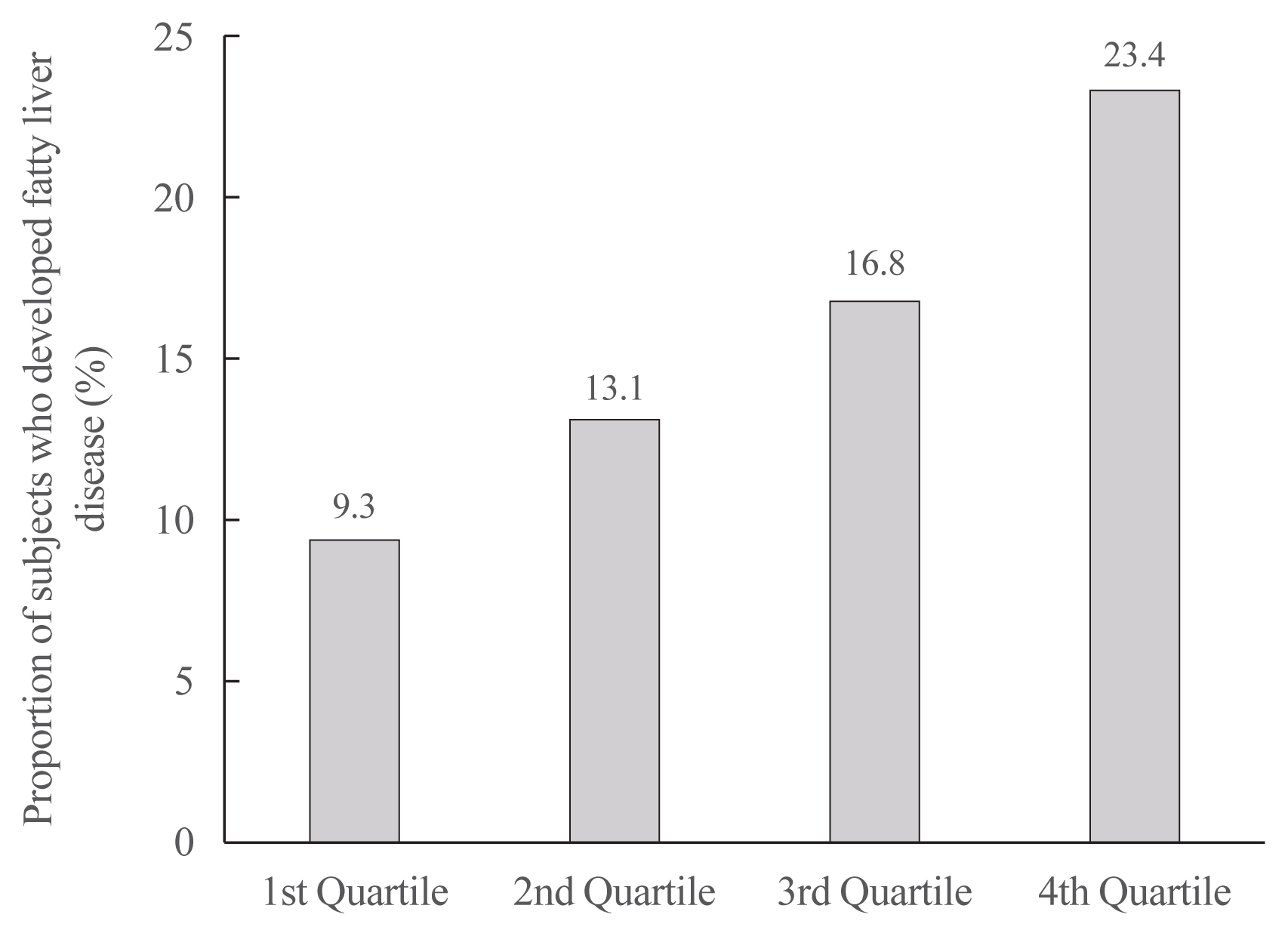
On dividing the participants into four groups according to ASVW quartile groups, those in the highest quartile showed a significantly increased risk of NAFLD compared to those in the lowest quartile (odds ratio [OR], 1.89; 95% confidence interval [CI], 1.63 to 2.19). Among participants without obesity at baseline, individuals with high ASVW showed increased risk of NAFLD (OR, 1.80; 95% CI, 1.61 to 2.01). Participants with increased weight over 4 years and high ASVW demonstrated higher risk of NAFLD compared to those with stable weight and low ASVW (OR, 4.87; 95% CI, 4.29 to 5.53).
Conclusion
Regardless of participant baseline obesity status, high weight variability was associated with an increased risk of developing NAFLD. Our results suggest that further effort is required to minimize weight fluctuations after achieving a desirable body weight.
-
Citations
Citations to this article as recorded by  - Changes in Macronutrients during Dieting Lead to Weight Cycling and Metabolic Complications in Mouse Model
Anouk Charlot, Anthony Bringolf, Léa Debrut, Joris Mallard, Anne-Laure Charles, Emilie Crouchet, Delphine Duteil, Bernard Geny, Joffrey Zoll
Nutrients.2024; 16(5): 646. CrossRef - Body weight variability and the risk of liver‐related outcomes in type 2 diabetes and steatotic liver disease: a cohort study
Nathalie C. Leite, Claudia R. L. Cardoso, Cristiane A. Villela‐Nogueira, Gil F. Salles
Obesity.2024;[Epub] CrossRef - Weight variability, physical functioning and incident disability in older adults
Katie J. McMenamin, Tamara B. Harris, Joshua F. Baker
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(4): 1648. CrossRef - Dulaglutide Ameliorates Palmitic Acid-Induced Hepatic Steatosis by Activating FAM3A Signaling Pathway
Jinmi Lee, Seok-Woo Hong, Min-Jeong Kim, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
Endocrinology and Metabolism.2022; 37(1): 74. CrossRef - Triglyceride and glucose index is a simple and easy‐to‐calculate marker associated with nonalcoholic fatty liver disease
Kyung‐Soo Kim, Sangmo Hong, Hong‐Yup Ahn, Cheol‐Young Park
Obesity.2022; 30(6): 1279. CrossRef - Metabolic (dysfunction)-associated fatty liver disease in individuals of normal weight
Mohammed Eslam, Hashem B. El-Serag, Sven Francque, Shiv K. Sarin, Lai Wei, Elisabetta Bugianesi, Jacob George
Nature Reviews Gastroenterology & Hepatology.2022; 19(10): 638. CrossRef - Impact of COVID-19 Lockdown on Non-Alcoholic Fatty Liver Disease and Insulin Resistance in Adults: A before and after Pandemic Lockdown Longitudinal Study
Ángel Arturo López-González, Bárbara Altisench Jané, Luis Masmiquel Comas, Sebastiana Arroyo Bote, Hilda María González San Miguel, José Ignacio Ramírez Manent
Nutrients.2022; 14(14): 2795. CrossRef - Higher Weight Variability Could Bring You a Fatty Liver
Yeoree Yang, Jae-Hyoung Cho
Endocrinology and Metabolism.2021; 36(4): 766. CrossRef - Autonomic Imbalance Increases the Risk for Non-alcoholic Fatty Liver Disease
Inha Jung, Da Young Lee, Mi Yeon Lee, Hyemi Kwon, Eun-Jung Rhee, Cheol-Young Park, Ki-Won Oh, Won-Young Lee, Sung-Woo Park, Se Eun Park
Frontiers in Endocrinology.2021;[Epub] CrossRef
- Endocrine Research
- Clusterin Protects Lipotoxicity-Induced Apoptosis via Upregulation of Autophagy in Insulin-Secreting Cells
-
Seok-Woo Hong, Jinmi Lee, Min Jeong Kim, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2020;35(4):943-953. Published online December 2, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.768
-
-
5,690
View
-
135
Download
-
4
Web of Science
-
7
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
There is a great need to discover factors that could protect pancreatic β-cells from apoptosis and thus prevent diabetes mellitus. Clusterin (CLU), a chaperone protein, plays an important role in cell protection in numerous cells and is involved in various cellular mechanisms, including autophagy. In the present study, we investigated the protective role of CLU through autophagy regulation in pancreatic β-cells.
Methods
To identify the protective role of CLU, mouse insulinoma 6 (MIN6) cells were incubated with CLU and/or free fatty acid (FFA) palmitate, and cellular apoptosis and autophagy were examined.
Results
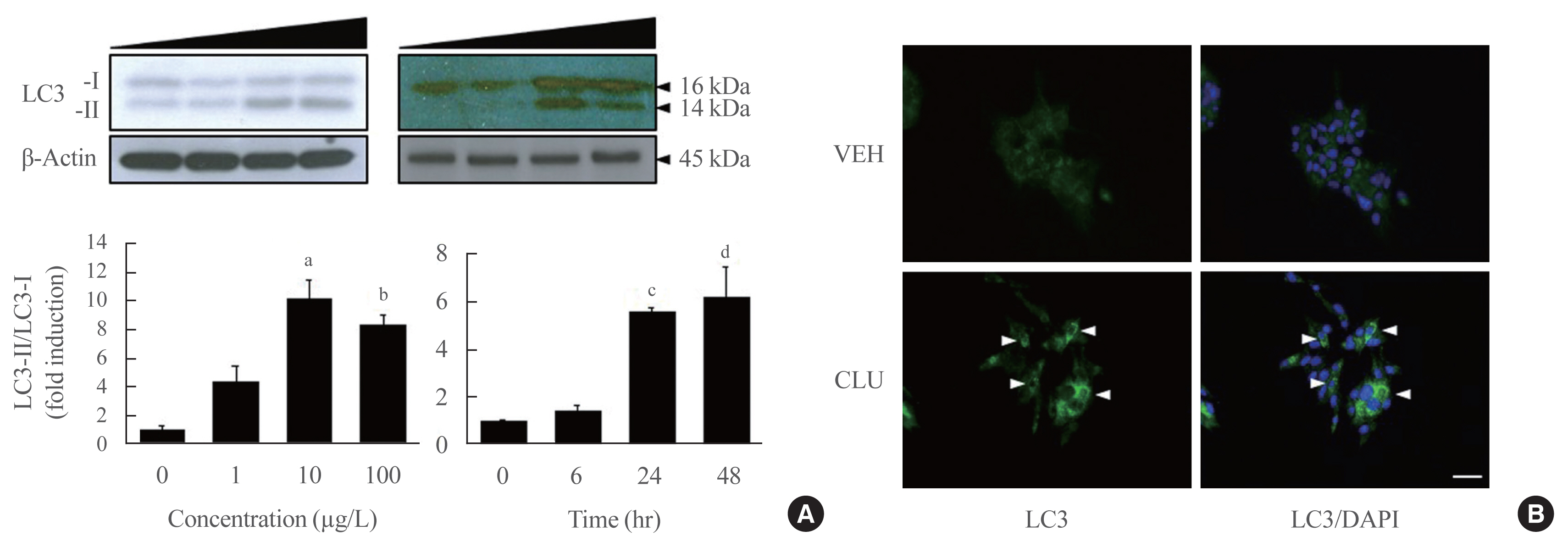
Treatment with CLU remarkably upregulated microtubule-associated protein 1-light chain 3 (LC3)-II conversion in a doseand time-dependent manner with a significant increase in the autophagy-related 3 (Atg3) gene expression level, which is a mediator of LC3-II conversion. Moreover, co-immunoprecipitation and fluorescence microscopy experiments showed that the molecular interaction of LC3 with Atg3 and p62 was markedly increased by CLU. Stimulation of LC3-II conversion by CLU persisted in lipotoxic conditions, and FFA-induced apoptosis and dysfunction were simultaneously improved by CLU treatment. Finally, inhibition of LC3-II conversion by Atg3 gene knockdown markedly attenuated the cytoprotective effect of CLU.
Conclusion
Taken together, these findings suggest that CLU protects pancreatic β-cells against lipotoxicity-induced apoptosis via autophagy stimulation mediated by facilitating LC3-II conversion. Thus, CLU has therapeutic effects on FFA-induced pancreatic β-cell dysfunction.
-
Citations
Citations to this article as recorded by  - Docosahexanoic Acid Attenuates Palmitate-Induced Apoptosis by Autophagy Upregulation via GPR120/mTOR Axis in Insulin-Secreting Cells
Seok-Woo Hong, Jinmi Lee, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
Endocrinology and Metabolism.2024; 39(2): 353. CrossRef - Exercise as a non-pharmacological intervention to protect pancreatic beta cells in individuals with type 1 and type 2 diabetes
Alexandra Coomans de Brachène, Corentin Scoubeau, Anyïshai E. Musuaya, Jose Maria Costa-Junior, Angela Castela, Julie Carpentier, Vitalie Faoro, Malgorzata Klass, Miriam Cnop, Decio L. Eizirik
Diabetologia.2023; 66(3): 450. CrossRef - Apolipoprotein J Attenuates Vascular Restenosis by Promoting Autophagy and Inhibiting the Proliferation and Migration of Vascular Smooth Muscle Cells
Ning Yang, Bo Dong, Yanqiu Song, Yang Li, Lu Kou, Qin Qin
Journal of Cardiovascular Translational Research.2022; 15(5): 1086. CrossRef - Targets for rescue from fatty acid-induced lipotoxicity in pancreatic beta cells
Seok-Woo Hong, Won-Young Lee
Cardiovascular Prevention and Pharmacotherapy.2022; 4(2): 57. CrossRef - Co-regulators of autophagy and the cell cycle in HFD − As treated mice
Marzieh Zeinvand-Lorestani, Mohammad Javad Khodayar, Ali Teimoori, Najmaldin Saki, Akram Ahangarpour, Ali Ranjbar, Hamed Zeinvand-Lorestani
Journal of Trace Elements and Minerals.2022; 2: 100018. CrossRef - Targeting pancreatic β cells for diabetes treatment
Chirag Jain, Ansarullah, Sara Bilekova, Heiko Lickert
Nature Metabolism.2022; 4(9): 1097. CrossRef - Mechanisms of Beta-Cell Apoptosis in Type 2 Diabetes-Prone Situations and Potential Protection by GLP-1-Based Therapies
Safia Costes, Gyslaine Bertrand, Magalie A. Ravier
International Journal of Molecular Sciences.2021; 22(10): 5303. CrossRef
- Clinical Study
- The Prevalence and Risk of Type 2 Diabetes in Adults with Disabilities in Korea
-
Inha Jung, Hyemi Kwon, Se Eun Park, Kyung-Do Han, Yong-Gyu Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2020;35(3):552-561. Published online July 22, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.653
-
-
8,133
View
-
188
Download
-
11
Web of Science
-
11
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
People with disabilities are at risk of secondary conditions such as diabetes. The aim of this study was to evaluate the prevalence and risk of type 2 diabetes in South Korea, especially among people with all types of disabilities.
Methods
We conducted a cross-sectional study using data from the Korean National Health Insurance Service, with two disabilityfree controls matched for each participant with disabilities by age and sex. Information regarding the type, severity and grade of disabilities was obtained based on the National Disability Registry. Diagnosis of type 2 diabetes was defined according to the following criteria: presence of International Classification of Diseases, Tenth Revision, Clinical Modification codes E11, E12, E13, or E14 and claims for at least one oral anti-diabetic agent or insulin at baseline, or fasting glucose level ≥126 mg/dL.
Results
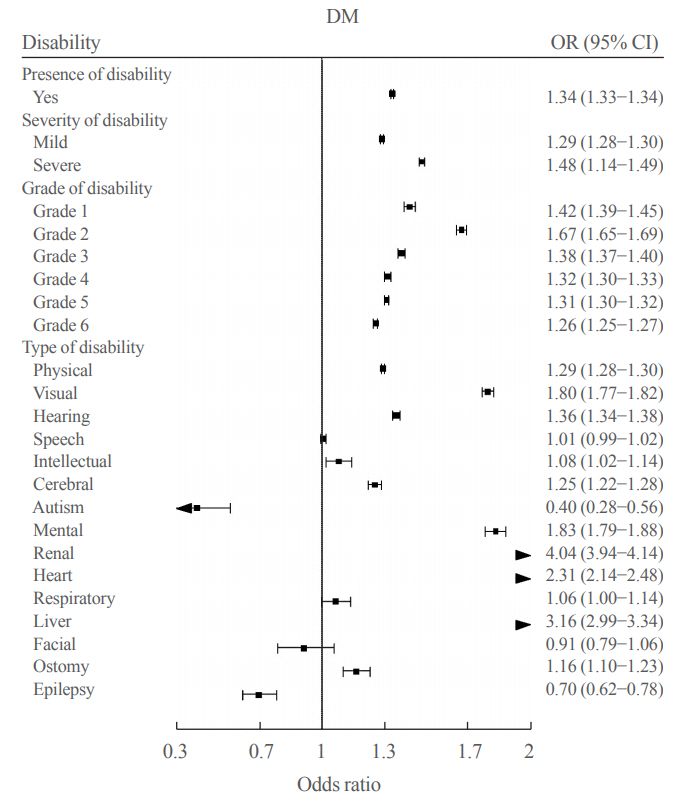
We included 1,297,806 participants with disabilities and 2,943,719 control. Out of 4,241,525 participants, 841,990 (19.9%) were diagnosed with diabetes. The prevalence of diabetes was higher in the disability group compared with individuals without disabilities (23.1% vs. 18.4%). The odds of having diabetes was higher in the disability group compared with the control group (adjusted odds ratio, 1.34; 95% confidence interval, 1.33 to 1.34). The results showed higher prevalence of diabetes in the mildly disabled group (23.2%) than in the severely disabled group (22.7%).
Conclusion
The prevalence and risk of diabetes were higher in people with disabilities compared with the general population. Physicians and public health authorities should focus on people with disabilities for proper diabetes management.
-
Citations
Citations to this article as recorded by  - Widening disparities in the national prevalence of diabetes mellitus for people with disabilities in South Korea
I. Hwang, S.Y. Kim, Y.Y. Kim, J.H. Park
Public Health.2024; 226: 173. CrossRef - Bipolar disorder and the risk of cardiometabolic diseases, heart failure, and all-cause mortality: a population-based matched cohort study in South Korea
You-Bin Lee, Hyewon Kim, Jungkuk Lee, Dongwoo Kang, Gyuri Kim, Sang-Man Jin, Jae Hyeon Kim, Hong Jin Jeon, Kyu Yeon Hur
Scientific Reports.2024;[Epub] CrossRef - Psychotic Disorders and the Risk of Type 2 Diabetes Mellitus, Atherosclerotic Cardiovascular Diseases, and All-Cause Mortality: A Population-Based Matched Cohort Study
You-Bin Lee, Hyewon Kim, Jungkuk Lee, Dongwoo Kang, Gyuri Kim, Sang-Man Jin, Jae Hyeon Kim, Hong Jin Jeon, Kyu Yeon Hur
Diabetes & Metabolism Journal.2024; 48(1): 122. CrossRef - Pathways linking health literacy to self-care in diabetic patients with physical disabilities: A moderated mediation model
Hye Jin Nam, Ju Young Yoon, Wen-Jun Tu
PLOS ONE.2024; 19(3): e0299971. CrossRef - Dysphagia Requiring Medical Attention in Parkinson’s Disease: A Korean Population-Based Study
Seungwoo Cha, Won Kee Chang, Hee-Mun Cho, Kyungdo Han, Nam-Jong Paik, Sohyun Kwon, Won-Seok Kim
Journal of Korean Medical Science.2023;[Epub] CrossRef - Disparities in diabetes-related avoidable hospitalization among diabetes patients with disability using a nationwide cohort study
Hin Moi Youn, Dong-Woo Choi, Sung-In Jang, Eun-Cheol Park
Scientific Reports.2022;[Epub] CrossRef - Disability type–specific mortality patterns and life expectancy among disabled people in South Korea using 10-year combined data between 2008 and 2017
Jinwook Bahk, Hee-Yeon Kang, Young-Ho Khang
Preventive Medicine Reports.2022; 29: 101958. CrossRef - Cholecystectomy reduces the risk of myocardial and cerebral infarction in patients with gallstone-related infection
Seon Mee Park, Hyun Jung Kim, Tae Uk Kang, Heather Swan, Hyeong Sik Ahn
Scientific Reports.2022;[Epub] CrossRef - Nationwide trends in the incidence of tuberculosis among people with disabilities in Korea:
a nationwide serial cross-sectional study
Jinsoo Min, So Young Kim, Jong Eun Park, Yeon Yong Kim, Jong Hyock Park
Epidemiology and Health.2022; 44: e2022098. CrossRef - Cumulative exposure to impaired fasting glucose and future risk of type 2 diabetes mellitus
Mee Kyoung Kim, Kyungdo Han, Eun Sil Koh, Oak-Kee Hong, Ki-Hyun Baek, Ki-Ho Song, Hyuk-Sang Kwon
Diabetes Research and Clinical Practice.2021; 175: 108799. CrossRef - Diabetes in People with Disabilities: a Call for Action
Inha Jung, Eun-Jung Rhee, Won-Young Lee
Cardiovascular Prevention and Pharmacotherapy.2021; 3(4): 82. CrossRef
- Clinical Study
- Serum Adiponectin and Progranulin Level in Patients with Benign Thyroid Nodule or Papillary Thyroid Cancer
-
Hyemi Kwon, Se Eun Park, Ji-Sup Yun, Cheol-Young Park
-
Endocrinol Metab. 2020;35(2):396-406. Published online June 24, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.2.396
-
-
5,657
View
-
109
Download
-
11
Web of Science
-
8
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Obesity is associated with thyroid cancer risk. Adiponectin has insulin-sensitizing and anti-inflammatory effects, while progranulin is associated with inflammation and tumorigenesis. We investigated serum adiponectin and progranulin levels in patients with benign thyroid nodule (benign group) and papillary thyroid cancer (PTC; PTC group). The associations between these levels and the clinicopathological features of PTC were evaluated.
Methods
We included 157 patients who underwent thyroid surgery (17% of benign and 83% of PTC group). Clinicopathological features including size, lymph node metastasis, extrathyroidal extension (ETE), multifocality, American Thyroid Association risk stratification were evaluated.
Results
The age was 42.0 years, and 69% were female. Serum adiponectin and progranulin levels were 6.3 μg/mL and 101.5 ng/mL in the benign group and 5.4 μg/mL and 106.1 ng/mL in the PTC group, respectively (P=0.6 and P=0.4, respectively). Serum adiponectin levels showed no significant differences according to clinicopathological features of PTC. The proportions of patients with primary tumor size >1 cm were 3%, 5%, 8%, and 8% according to serum progranulin level quartiles, respectively (P=0.03). The proportions of patients with microscopic/gross ETE were 8%/0%, 9%/1%, 11%/1%, and 11%/2% according to serum progranulin level quartiles, respectively. Median serum progranulin level was significantly higher in patients with PTC >1 cm than in patients with papillary thyroid microcarcinoma (P=0.04, 115.3 ng/mL and 104.7 ng/mL, respectively).
Conclusion
Serum adiponectin and progranulin levels showed no significant difference between benign and PTC groups. Increased serum progranulin levels were significantly associated with PTC >1 cm and microscopic and gross ETE.
-
Citations
Citations to this article as recorded by  - Exploring the logic and conducting a comprehensive evaluation of AdipoRon-based adiponectin replacement therapy against hormone-related cancers—a systematic review
Lucas Fornari Laurindo, Andreline Franchi Sosin, Caroline Barbalho Lamas, Ricardo de Alvares Goulart, Jesselina Francisco dos Santos Haber, Claudia Rucco Penteado Detregiachi, Sandra Maria Barbalho
Naunyn-Schmiedeberg's Archives of Pharmacology.2024; 397(4): 2067. CrossRef - Adiponectin Inhibits the Progression of Obesity-Associated Papillary Thyroid Carcinoma Through Autophagy
Changlin Li, Jiao Zhang, Gianlorenzo Dionigi, Nan Liang, Haixia Guan, Hui Sun
Endocrinology.2024;[Epub] CrossRef - Progranulin Oncogenic Network in Solid Tumors
Elisa Ventura, Giacomo Ducci, Reyes Benot Dominguez, Valentina Ruggiero, Antonino Belfiore, Elena Sacco, Marco Vanoni, Renato V. Iozzo, Antonio Giordano, Andrea Morrione
Cancers.2023; 15(6): 1706. CrossRef - Obesity and thyroid cancer risk
Lauren C. Burrage, Donald S.A. McLeod, Susan J. Jordan
Current Opinion in Endocrinology, Diabetes & Obesity.2023; 30(5): 244. CrossRef - Progranulin promoted the proliferation, metastasis, and suppressed apoptosis via JAK2-STAT3/4 signaling pathway in papillary thyroid carcinoma
Yanxu Dong, Hao Tan, Lidong Wang, Zhen Liu
Cancer Cell International.2023;[Epub] CrossRef - Obesity and Thyroid Cancer Risk: An Update
Fabiana Franchini, Giuseppe Palatucci, Annamaria Colao, Paola Ungaro, Paolo Emidio Macchia, Immacolata Cristina Nettore
International Journal of Environmental Research and Public Health.2022; 19(3): 1116. CrossRef - Obesity and Overweight Are Associated with Minimal Extrathyroidal Extension, Multifocality and Bilaterality of Papillary Thyroid Cancer
Krzysztof Kaliszewski, Dorota Diakowska, Marta Rzeszutko, Jerzy Rudnicki
Journal of Clinical Medicine.2021; 10(5): 970. CrossRef - Adiponectin and Thyroid Cancer: Insight into the Association between Adiponectin and Obesity
Yuanyuan Zhou, Ying Yang, Taicheng Zhou, Bai Li, Zhanjian Wang
Aging and disease.2021; 12(2): 597. CrossRef
- Clinical Study
- Visceral-to-Subcutaneous Abdominal Fat Ratio Is Associated with Nonalcoholic Fatty Liver Disease and Liver Fibrosis
-
Chan-Hee Jung, Eun-Jung Rhee, Hyemi Kwon, Yoosoo Chang, Seungho Ryu, Won-Young Lee
-
Endocrinol Metab. 2020;35(1):165-176. Published online March 19, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.1.165
-
-
6,562
View
-
137
Download
-
26
Web of Science
-
27
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
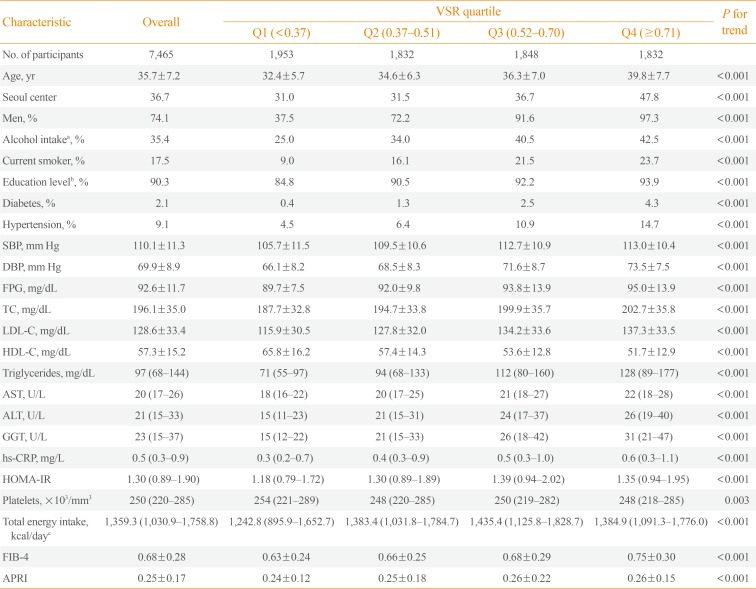
We evaluated the association of visceral-to-subcutaneous fat ratio (VSR) with nonalcoholic fatty liver disease (NAFLD) and advanced fibrosis degree based on noninvasive serum fibrosis markers in the general population with NAFLD. MethodsThis is a cross-sectional study, in 7,465 Korean adults who underwent health screening examinations. NAFLD was defined as fatty liver detected on ultrasonography, and visceral and subcutaneous abdominal fat was measured using computed tomography. We predicted fibrosis based on the fibrosis-4 (FIB-4) score and aspartate aminotransferase-to-platelet ratio index (APRI) and categorized the risk for advanced fibrosis as low, indeterminate, or high. ResultsThe multivariable-adjusted prevalence ratios for indeterminate to high risk of advanced fibrosis based on FIB-4, determined by comparing the second, third, and fourth quartiles with the first quartile of VSR, were 3.38 (95% confidence interval [CI], 0.64 to 17.97), 9.41 (95% CI, 1.97 to 45.01), and 19.34 (95% CI, 4.06 to 92.18), respectively. The multivariable-adjusted prevalence ratios for intermediate to high degree of fibrosis according to APRI also increased across VSR quartiles (5.04 [95% CI, 2.65 to 9.59], 7.51 [95% CI, 3.91 to 14.42], and 19.55 [95% CI, 9.97 to 38.34], respectively). High VSR was more strongly associated with the prevalence of NAFLD in nonobese subjects than in obese subjects, and the associations between VSR and intermediate to high probability of advanced fibrosis in NAFLD were stronger in obese subjects than in nonobese subjects. ConclusionHigh VSR values predicted increased NAFLD risk and advanced fibrosis risk with NAFLD, and the predictive value of VSR for indeterminate to high risk of advanced fibrosis was higher in obese subjects than in nonobese subjects.
-
Citations
Citations to this article as recorded by  - Opportunistic Extraction of Quantitative CT Biomarkers: Turning the Incidental Into Prognostic Information
Mohammad Nazri Md Shah, Raja Rizal Azman, Wai Yee Chan, Kwan Hoong Ng
Canadian Association of Radiologists Journal.2024; 75(1): 92. CrossRef - Positive Association Between the Chinese Visceral Adiposity Index and Nonalcoholic Fatty Liver Disease in Lean Adults
Shuxia Shen, Hangkai Huang, Jinghua Wang, Zexi Tang, Chao Shen, Chengfu Xu
Digestive Diseases and Sciences.2023; 68(2): 656. CrossRef - Association between Sarcopenic Obesity Status and Nonalcoholic Fatty Liver Disease and Fibrosis
Wolhwa Song, Sung Hwan Yoo, Jinsun Jang, Su Jung Baik, Byoung Kwon Lee, Hyun Woong Lee, Jong Suk Park
Gut and Liver.2023; 17(1): 130. CrossRef - Using hyperhomocysteinemia and body composition to predict the risk of non-alcoholic fatty liver disease in healthcare workers
Xiaoyan Hao, Honghai He, Liyuan Tao, Peng Wang
Frontiers in Endocrinology.2023;[Epub] CrossRef - Visceral and subcutaneous fat, muscle mass, and liver volume as noninvasive predictors of the progress of non-alcoholic fatty liver disease
Omar M. Mahmoud, Gehad Abd Elaziz Mahmoud, Haisam Atta, Wael A. Abbas, Hanan M. Ahmed, Mohamed A. A. Abozaid
Egyptian Journal of Radiology and Nuclear Medicine.2023;[Epub] CrossRef - Relationship between metabolic associated fatty liver disease and body fat ratio, visceral fat area, and resting metabolic rate estimated by bioelectrical impedance analysis
Deng-Hua He, Yong-Zhan Zhang, Liang Xu, Jia-Jia Pei, Ying Zhang, Zhong-Fang Yan
World Chinese Journal of Digestology.2023; 31(2): 56. CrossRef - Poor glycaemic control and ectopic fat deposition mediates the increased risk of non-alcoholic steatohepatitis in high-risk populations with type 2 diabetes: Insights from Bayesian-network modelling
T. Waddell, A. Namburete, P. Duckworth, A. Fichera, A. Telford, H. Thomaides-Brears, D. J. Cuthbertson, M. Brady
Frontiers in Endocrinology.2023;[Epub] CrossRef - Metabolic Dysfunction-Associated Fatty Liver Disease and Mortality: A Population-Based Cohort Study
Kyung-Soo Kim, Sangmo Hong, Hong-Yup Ahn, Cheol-Young Park
Diabetes & Metabolism Journal.2023; 47(2): 220. CrossRef - Subcutaneous Fat Obesity in a High Body Mass Index Donor Is Not a Contraindication to Living Donor Hepatectomy
Hirak Pahari, Amey Sonavane, Amruth Raj, Anup Kumar Agrawal, Ambreen Sawant, Deepak Kumar Gupta, Amit Gharat, Vikram Raut, Sorabh Kapoor
Case Reports in Hepatology.2023; 2023: 1. CrossRef - Comparison of cardiometabolic risk factors between obese and non-obese patients with nonalcoholic fatty liver disease
Zahra Yari, Danial Fotros, Azita Hekmatdoost
Scientific Reports.2023;[Epub] CrossRef - Association of Visceral Fat Obesity, Sarcopenia, and Myosteatosis with Non-Alcoholic Fatty Liver Disease without Obesity
Hong-Kyu Kim, Sung-Jin Bae, Min Jung Lee, Eun Hee Kim, Hana Park, Hwi Seung Kim, Yun Kyung Cho, Chang Hee Jung, Woo Je Lee, Jaewon Choe
Clinical and Molecular Hepatology.2023; 29(4): 987. CrossRef - Visceral Adipose Tissue Inflammation and Radiographic Visceral-to-Subcutaneous Adipose Tissue Ratio in Patients with Cirrhosis
Nghiem B. Ha, Soo-Jin Cho, Yara Mohamad, Dorothea Kent, Grace Jun, Randi Wong, Vivek Swarnakar, Shezhang Lin, Jacquelyn J. Maher, Jennifer C. Lai
Digestive Diseases and Sciences.2022; 67(7): 3436. CrossRef - The Influence of Obesity and Metabolic Health on Vascular Health
Eun-Jung Rhee
Endocrinology and Metabolism.2022; 37(1): 1. CrossRef - The effect of combined exercises on the plasma levels of retinol-binding protein 4 and its relationship with insulin resistance and hepatic fat content in postmenopausal women with nonalcoholic fatty liver disease
Masoumeh NOROUZPOUR, Sayyed M. MARANDI, Mohsen GHANBARZADEH, Abbasali ZARE MAIVAN
The Journal of Sports Medicine and Physical Fitness.2022;[Epub] CrossRef - The Perirenal Fat Thickness Was Associated with Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Mellitus
Yuxian Yang, Shuting Li, Yuechao Xu, Jing Ke, Dong Zhao
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2022; Volume 15: 1505. CrossRef - Visceral adiposity is an independent risk factor for high intra-operative blood loss during living-donor liver transplantation; could preoperative rehabilitation and nutritional therapy mitigate that risk?
Mahmoud Macshut, Toshimi Kaido, Siyuan Yao, Yosuke Miyachi, Mohamed Sharshar, Sena Iwamura, Masaaki Hirata, Hisaya Shirai, Naoko Kamo, Shintaro Yagi, Shinji Uemoto
Clinical Nutrition.2021; 40(3): 956. CrossRef - A review of non‐alcoholic fatty liver disease in non‐obese and lean individuals
Mitra Ahadi, Kasra Molooghi, Negin Masoudifar, Ali Beheshti Namdar, Hassan Vossoughinia, Mohammadreza Farzanehfar
Journal of Gastroenterology and Hepatology.2021; 36(6): 1497. CrossRef - Quantification of abdominal fat from computed tomography using deep learning and its association with electronic health records in an academic biobank
Matthew T MacLean, Qasim Jehangir, Marijana Vujkovic, Yi-An Ko, Harold Litt, Arijitt Borthakur, Hersh Sagreiya, Mark Rosen, David A Mankoff, Mitchell D Schnall, Haochang Shou, Julio Chirinos, Scott M Damrauer, Drew A Torigian, Rotonya Carr, Daniel J Rader
Journal of the American Medical Informatics Association.2021; 28(6): 1178. CrossRef - Hepatic Steatosis in Patients With Single Ventricle and a Fontan Circulation
David A. Katz, Daniel Peck, Adam M. Lubert, Mathias Possner, Faizeen Zafar, Andrew T. Trout, Joseph J. Palermo, Nadeem Anwar, Jonathan R. Dillman, Adam W. Powell, Stavra A. Xanthakos, Alexander R. Opotowsky, Gruschen Veldtman, Tarek Alsaied
Journal of the American Heart Association.2021;[Epub] CrossRef - Superficial vs Deep Subcutaneous Adipose Tissue: Sex-Specific Associations With Hepatic Steatosis and Metabolic Traits
Tessa Brand, Inge Christina Lamberta van den Munckhof, Marinette van der Graaf, Kiki Schraa, Helena Maria Dekker, Leonardus Antonius Bernardus Joosten, Mihai Gheorghe Netea, Niels Peter Riksen, Jacqueline de Graaf, Joseph Henricus Wilhelmus Rutten
The Journal of Clinical Endocrinology & Metabolism.2021; 106(10): e3881. CrossRef - Baseline homeostasis model assessment of insulin resistance associated with fibrosis progression in patients with nonalcoholic fatty liver disease without diabetes: A cohort study
Dae-Jeong Koo, Mi Yeon Lee, Inha Jung, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee, Ming-Lung Yu
PLOS ONE.2021; 16(8): e0255535. CrossRef - Randomised clinical trial: semaglutide versus placebo reduced liver steatosis but not liver stiffness in subjects with non‐alcoholic fatty liver disease assessed by magnetic resonance imaging
Anne Flint, Grit Andersen, Paul Hockings, Lars Johansson, Anni Morsing, Mads Sundby Palle, Thomas Vogl, Rohit Loomba, Leona Plum‐Mörschel
Alimentary Pharmacology & Therapeutics.2021; 54(9): 1150. CrossRef - Effects of IL-33 on 3T3-L1 cells and obese mice models induced by a high-fat diet
Yue Kai, Jingtao Gao, Hu Liu, Yubing Wang, Chenrui Tian, Sheng Guo, Ling He, Min Li, Zhongwei Tian, Xiangfeng Song
International Immunopharmacology.2021; 101: 108209. CrossRef - Lipid Accumulation Product as an Index for Visceral Obesity and Cardiovascular Risk among a Sample of Obese Egyptian Women
Nayera E. Hassan, Sahar A. El-Masry, Gamila S. M. El-Saeed, Mohamed S. El Hussieny
Open Access Macedonian Journal of Medical Sciences.2021; 9(B): 1229. CrossRef - Combined Effects of Dyslipidemia and High Adiposity on the Estimated Glomerular Filtration Rate in a Middle-Aged Chinese Population
Xichang Wang, Haoyu Wang, Jiashu Li, Xiaotong Gao, Yutong Han, Weiping Teng, Zhongyan Shan, Yaxin Lai
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2021; Volume 14: 4513. CrossRef - Determination of “indeterminate score” measurements in lean nonalcoholic fatty liver disease patients from western Saudi Arabia
Yasir Mohammed Khayyat
World Journal of Hepatology.2021; 13(12): 2150. CrossRef - Utility of Liver Function Tests and Fatty Liver Index to Categorize Metabolic Phenotypes in a Mediterranean Population
Dariusz Narankiewicz, Josefina Ruiz-Nava, Veronica Buonaiuto, María Isabel Ruiz-Moreno, María Dolores López-Carmona, Luis Miguel Pérez-Belmonte, Ricardo Gómez-Huelgas, María Rosa Bernal-López
International Journal of Environmental Research and Public Health.2020; 17(10): 3518. CrossRef
- Endocrine Research
- Deficiency of Sphingosine-1-Phosphate Reduces the Expression of Prohibitin and Causes β-Cell Impairment via Mitochondrial Dysregulation
-
Seok-Woo Hong, Jinmi Lee, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Cheol-Young Park, Ki-Won Oh, Sung-Woo Park, Won-Young Lee
-
Endocrinol Metab. 2018;33(3):403-412. Published online September 18, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.3.403
-
-
4,232
View
-
50
Download
-
16
Web of Science
-
16
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Emerging evidence suggests that sphingolipids may be involved in type 2 diabetes. However, the exact signaling defect through which disordered sphingolipid metabolism induces β-cell dysfunction remains unknown. The current study demonstrated that sphingosine-1-phosphate (S1P), the product of sphingosine kinase (SphK), is an essential factor for maintaining β-cell function and survival via regulation of mitochondrial action, as mediated by prohibitin (PHB). MethodsWe examined β-cell function and viability, as measured by mitochondrial function, in mouse insulinoma 6 (MIN6) cells in response to manipulation of cellular S1P and PHB levels. ResultsLack of S1P induced by sphingosine kinase inhibitor (SphKi) treatment caused β-cell dysfunction and apoptosis, with repression of mitochondrial function shown by decreases in cellular adenosine triphosphate content, the oxygen consumption rate, the expression of oxidative phosphorylation complexes, the mitochondrial membrane potential, and the expression of key regulators of mitochondrial dynamics (mitochondrial dynamin-like GTPase [OPA1] and mitofusin 1 [MFN1]). Supplementation of S1P led to the recovery of mitochondrial function and greatly improved β-cell function and viability. Knockdown of SphK2 using small interfering RNA induced mitochondrial dysfunction, decreased glucose-stimulated insulin secretion (GSIS), and reduced the expression of PHB, an essential regulator of mitochondrial metabolism. PHB deficiency significantly reduced GSIS and induced mitochondrial dysfunction, and co-treatment with S1P did not reverse these trends. ConclusionAltogether, these data suggest that S1P is an essential factor in the maintenance of β-cell function and survival through its regulation of mitochondrial action and PHB expression.
-
Citations
Citations to this article as recorded by  - Mitochondrial Cristae Morphology Reflecting Metabolism, Superoxide Formation, Redox Homeostasis, and Pathology
Petr Ježek, Martin Jabůrek, Blanka Holendová, Hana Engstová, Andrea Dlasková
Antioxidants & Redox Signaling.2023; 39(10-12): 635. CrossRef - Sphingolipids in mitochondria—from function to disease
Maryam Jamil, Lauren Ashley Cowart
Frontiers in Cell and Developmental Biology.2023;[Epub] CrossRef - Sphingosine‐1‐phosphate in mitochondrial function and metabolic diseases
Meng Duan, Pan Gao, Sheng‐xi Chen, Petr Novák, Kai Yin, Xiao Zhu
Obesity Reviews.2022;[Epub] CrossRef - Involvement of miR‐27a‐3p in diabetic nephropathy via affecting renal fibrosis, mitochondrial dysfunction, and endoplasmic reticulum stress
Lina Wu, Qingzhu Wang, Feng Guo, Xiaojun Ma, Jiao Wang, Yanyan Zhao, Yushan Yan, Guijun Qin
Journal of Cellular Physiology.2021; 236(2): 1454. CrossRef - Sphingosine‐1‐phosphate in acute exercise and training
Katarzyna Hodun, Adrian Chabowski, Marcin Baranowski
Scandinavian Journal of Medicine & Science in Sports.2021; 31(5): 945. CrossRef - The Ethyl Acetate Extract From Celastrus orbiculatus Promotes Apoptosis of Gastric Cancer Cells Through Mitochondria Regulation by PHB
Lide Tao, Zixin Yin, Tengyang Ni, Zewen Chu, Shihua Hao, Zeyu Wang, Masataka Sunagawa, Haibo Wang, Yanqing Liu
Frontiers in Pharmacology.2021;[Epub] CrossRef - Sphingosine 1-phosphate Stimulates Insulin Secretion and Improves Cell Survival by Blocking Voltage-dependent K+ Channels in β Cells
Zhihong Liu, Huanhuan Yang, Linping Zhi, Huan Xue, Zhihong Lu, Yanli Zhao, Lijuan Cui, Tao Liu, Shouan Ren, Peifeng He, Yunfeng Liu, Yi Zhang
Frontiers in Pharmacology.2021;[Epub] CrossRef - Sphingosine-1 Phosphate Lyase Regulates Sensitivity of Pancreatic Beta-Cells to Lipotoxicity
Yadi Tang, Thomas Plötz, Markus H. Gräler, Ewa Gurgul-Convey
International Journal of Molecular Sciences.2021; 22(19): 10893. CrossRef - Sphingolipids and Mitochondrial Dynamic
Lais Brigliadori Fugio, Fernanda B. Coeli-Lacchini, Andréia Machado Leopoldino
Cells.2020; 9(3): 581. CrossRef - Diminished Sphingolipid Metabolism, a Hallmark of Future Type 2 Diabetes Pathogenesis, Is Linked to Pancreatic β Cell Dysfunction
Saifur R. Khan, Yousef Manialawy, Andreea Obersterescu, Brian J. Cox, Erica P. Gunderson, Michael B. Wheeler
iScience.2020; 23(10): 101566. CrossRef - Neuronal Metabolism and Neuroprotection: Neuroprotective Effect of Fingolimod on Menadione-Induced Mitochondrial Damage
Antonio Gil, Elisa Martín-Montañez, Nadia Valverde, Estrella Lara, Federica Boraldi, Silvia Claros, Silvana-Yanina Romero-Zerbo, Oscar Fernández, Jose Pavia, Maria Garcia-Fernandez
Cells.2020; 10(1): 34. CrossRef - WITHDRAWN: Ceramide and Sphingosine 1-Phosphate in adipose dysfunction
Zijian Fang, Susan Pyne, Nigel J. Pyne
Progress in Lipid Research.2019; : 100991. CrossRef - Dynamic of mitochondrial network, cristae, and mitochondrial nucleoids in pancreatic β-cells
Petr Ježek, Andrea Dlasková
Mitochondrion.2019; 49: 245. CrossRef - Sphingosine kinase 1 overexpression induces MFN2 fragmentation and alters mitochondrial matrix Ca2+ handling in HeLa cells
I. Pulli, C. Löf, T. Blom, M.Y. Asghar, T. Lassila, N. Bäck, K.-L. Lin, J.H. Nyström, K. Kemppainen, D.M. Toivola, E. Dufour, A. Sanz, H.M. Cooper, J.B. Parys, K. Törnquist
Biochimica et Biophysica Acta (BBA) - Molecular Cell Research.2019; 1866(9): 1475. CrossRef - Ceramide and sphingosine 1-phosphate in adipose dysfunction
Zijian Fang, Susan Pyne, Nigel J. Pyne
Progress in Lipid Research.2019; 74: 145. CrossRef - S1P/S1P Receptor Signaling in Neuromuscolar Disorders
Elisabetta Meacci, Mercedes Garcia-Gil
International Journal of Molecular Sciences.2019; 20(24): 6364. CrossRef
- Thyroid
- Prevalence and Annual Incidence of Thyroid Disease in Korea from 2006 to 2015: A Nationwide Population-Based Cohort Study
-
Hyemi Kwon, Jin-hyung Jung, Kyung-Do Han, Yong-Gyu Park, Jung-Hwan Cho, Da Young Lee, Ji Min Han, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
-
Endocrinol Metab. 2018;33(2):260-267. Published online June 21, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.2.260
-
-
6,484
View
-
128
Download
-
37
Web of Science
-
37
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
The incidence of thyroid nodules has increased worldwide in recent years. Thyroid dysfunction is a potential risk factor for hypercholesterolemia, cardiovascular disease, osteoporosis, arrhythmia, and neuropsychiatric disease. This study investigated the prevalence and annual incidence of thyroid nodules, hypothyroidism, and hyperthyroidism in Koreans. MethodsIn this nationwide population-based cohort study, 51,834,660 subjects were included using the National Health Information database from 2006 to 2015, after the exclusion of subjects with thyroid cancer. ResultsThe prevalence in Korea in 2015 of thyroid nodules, hypothyroidism in patients taking thyroid hormone, and hyperthyroidism in patients undergoing treatment was 15.82/1,000 population, 15.94/1,000 population, and 2.76/1,000 population, respectively. All these diseases were more prevalent among women than among men. The number of incident cases of these three thyroid diseases steadily increased from 2006 to 2012, and then decreased through 2015. The incidence of thyroid nodules, hypothyroidism treated with thyroid hormone, and treated hyperthyroidism was 6.79/1,000 population, 1.76/1,000 population, and 0.55/1,000 population, respectively, in Korea in 2015. The use of methimazole continuously increased, from 33% of total antithyroid drug prescriptions in 2006 to 74.4% in 2015, and it became the most frequently prescribed antithyroid drug in Korea. In contrast, the use of propylthiouracil continuously decreased. ConclusionThis was the first nationwide study of the prevalence and annual incidence of thyroid nodules, hypothyroidism, and hyperthyroidism to take into account recent changes and to include the current status of patients receiving treatment.
-
Citations
Citations to this article as recorded by  - New-onset atrial fibrillation in seropositive rheumatoid arthritis: association with disease-modifying anti-rheumatic drugs treatment
Hyung Woo Kim, Minkyung Han, Inkyung Jung, Sung Soo Ahn
Rheumatology.2024; 63(3): 630. CrossRef - Nonalcoholic Fatty Liver Disease and the Risk of Thyroid Cancer Among Young Adults in South Korea
Hyemi Kwon, Kyung-Do Han, Sun Joon Moon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
The Journal of Clinical Endocrinology & Metabolism.2024; 109(3): e1095. CrossRef - Endocrine and metabolic comorbidities in primary cicatricial alopecia: A nationwide population‐based study
Da‐Ae Yu, Seong Rae Kim, Soo Ick Cho, Ohsang Kwon
The Journal of Dermatology.2024; 51(3): 429. CrossRef - Risk of non-thyroidal autoimmune diseases in patients with Graves’ disease: a nationwide retrospective cohort study
Seo Young Sohn, Jiyeon Ahn, Min Kyung Lee, Jae Hyuk Lee, Ji-Won Kwon, Ji-Min Kweon, Ju-Yeun Lee
Rheumatology.2024;[Epub] CrossRef - Cancer Risk in Graves Disease with Radioactive131I Treatment: A Nationwide Cohort Study
Kyeong Jin Kim, Jimi Choi, Kyoung Jin Kim, Eyun Song, Ji Hee Yu, Nam Hoon Kim, Hye Jin Yoo, Ji A Seo, Nan Hee Kim, Kyung Mook Choi, Sei Hyun Baik, Sin Gon Kim
Journal of Nuclear Medicine.2024; 65(5): 693. CrossRef - Long-term Effect of Thyrotropin-binding Inhibitor Immunoglobulin on Atrial Fibrillation in Euthyroid Patients
Jung-Chi Hsu, Kang-Chih Fan, Ting-Chuan Wang, Shu-Lin Chuang, Ying-Ting Chao, Ting-Tse Lin, Kuan-Chih Huang, Lian-Yu Lin, Lung-Chun Lin
Endocrine Practice.2024;[Epub] CrossRef - Myotonic dystrophy type 1 in South Korea: a comprehensive analysis of cancer and comorbidity risks
Incheol Seo, Jin-Mo Park
Neurological Sciences.2024;[Epub] CrossRef - Association of ITM2A rs1751094 polymorphism on X chromosome in Korean pediatric patients with autoimmune thyroid disease
Won K. Cho, In‐Cheol Baek, Sung E. Kim, Mirae Kim, Tai‐Gyu Kim, Byung‐Kyu Suh
Immunity, Inflammation and Disease.2023;[Epub] CrossRef - Preoperative Risk Stratification of Follicular-patterned Thyroid Lesions on Core Needle Biopsy by Histologic Subtyping and RAS Variant-specific Immunohistochemistry
Meejeong Kim, Sora Jeon, Chan Kwon Jung
Endocrine Pathology.2023; 34(2): 247. CrossRef - Cancer and Mortality Risks of Graves’ Disease in South Korea Based on National Data from 2010 to 2019
Young Ju Choi, Kyungdo Han, Won Kyoung Cho, Min Ho Jung, Byung-Kyu Suh
Clinical Epidemiology.2023; Volume 15: 535. CrossRef - Acromegaly and the long-term fracture risk of the vertebra and hip: a national cohort study
Hyemi Kwon, Kyung-Do Han, Bong-Sung Kim, Sun Joon Moon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
Osteoporosis International.2023; 34(9): 1591. CrossRef - Association of Thyroid Hormone Medication Adherence With Risk of Dementia
Saemi Han, Seogsong Jeong, Seulggie Choi, Sun Jae Park, Kyae Hyung Kim, Gyeongsil Lee, Yoosun Cho, Joung Sik Son, Sang Min Park
The Journal of Clinical Endocrinology & Metabolism.2023; 109(1): e225. CrossRef - Increased risk of incident gout in patients with hyperthyroidism: a nationwide retrospective cohort study
Ju-Yeun Lee, So-Yeon Park, Seo Young Sohn
Rheumatology International.2023; 44(3): 451. CrossRef - The Current Status of Hyperthyroidism in Korea
Hyemi Kwon
Endocrinology and Metabolism.2023; 38(4): 392. CrossRef - Prevalence, Treatment Status, and Comorbidities of Hyperthyroidism in Korea from 2003 to 2018: A Nationwide Population Study
Hwa Young Ahn, Sun Wook Cho, Mi Young Lee, Young Joo Park, Bon Seok Koo, Hang-Seok Chang, Ka Hee Yi
Endocrinology and Metabolism.2023; 38(4): 436. CrossRef - Comprehensive analysis of chemokine gene polymorphisms in Korean children with autoimmune thyroid disease
Chungwoo Shin, In-Cheol Baek, Won Kyoung Cho, Tai-Gyu Kim, Byung-Kyu Suh
Scientific Reports.2023;[Epub] CrossRef - Analysis of the status of treatment of benign thyroid diseases — a public health problem aggravated in the COVID-19 pandemic era
Giulianno Molina Melo, Antonio José Gonçalves, Fernando Walder, Carolina Ferraz, Murilo Catafesta Neves, Marcio Abrahão, Onivaldo Cervantes
Brazilian Journal of Otorhinolaryngology.2022; 88(6): 982. CrossRef - Graves’ disease and the risk of Parkinson’s disease: a Korean population-based study
Yoon Young Cho, Bongseong Kim, Dong Wook Shin, Jinyoung Youn, Ji Oh Mok, Chul-Hee Kim, Sun Wook Kim, Jae Hoon Chung, Kyungdo Han, Tae Hyuk Kim
Brain Communications.2022;[Epub] CrossRef - Graves’ Disease and the Risk of End-Stage Renal Disease: A Korean Population-Based Study
Yoon Young Cho, Bongseong Kim, Dong Wook Shin, Hye Ryoun Jang, Bo-Yeon Kim, Chan-Hee Jung, Jae Hyeon Kim, Sun Wook Kim, Jae Hoon Chung, Kyungdo Han, Tae Hyuk Kim
Endocrinology and Metabolism.2022; 37(2): 281. CrossRef - Incidence of hypothyroidism after treatment for breast cancer: A Korean population-based study
Jongmoo Park, Choongrak Kim, Yongkan Ki, Wontaek Kim, Jiho Nam, Donghyun Kim, Dahl Park, Hosang Jeon, Dong Woon Kim, Ji Hyeon Joo, Claudio Andaloro
PLOS ONE.2022; 17(6): e0269893. CrossRef - Genome-wide association study of hyperthyroidism based on electronic medical record from Taiwan
Ting-Yuan Liu, Wen-Ling Liao, Tzu-Yuan Wang, Chia-Jung Chan, Jan-Gowth Chang, Yu-Chia Chen, Hsing-Fang Lu, Hsien-Hui Yang, Shih-Yin Chen, Fuu-Jen Tsai
Frontiers in Medicine.2022;[Epub] CrossRef - Graves’ disease, its treatments, and the risk of atrial fibrillation: A Korean population-based study
Yoon Young Cho, Bongseong Kim, Dughyun Choi, Chul-Hee Kim, Dong Wook Shin, Jee Soo Kim, Seung-Jung Park, Sun Wook Kim, Jae Hoon Chung, Kyungdo Han, Tae Hyuk Kim
Frontiers in Endocrinology.2022;[Epub] CrossRef - Risk of autoimmune diseases in recurrent aphthous ulcer patients: A nationwide population study
Young Chan Lee, Su Jin Jeong, Young‐Gyu Eun, Ran Song, In‐Hwan Oh
Oral Diseases.2021; 27(6): 1443. CrossRef - Hyperthyroidism Prevalence in China After Universal Salt Iodization
Chuyuan Wang, Yongze Li, Di Teng, Xiaoguang Shi, Jianming Ba, Bing Chen, Jianling Du, Lanjie He, Xiaoyang Lai, Yanbo Li, Haiyi Chi, Eryuan Liao, Chao Liu, Libin Liu, Guijun Qin, Yingfen Qin, Huibiao Quan, Bingyin Shi, Hui Sun, Xulei Tang, Nanwei Tong, Gui
Frontiers in Endocrinology.2021;[Epub] CrossRef - Comorbidity network analysis related to obesity in middle-aged and older adults: findings from Korean population-based survey data
Hye Ah Lee, Hyesook Park
Epidemiology and Health.2021; 43: e2021018. CrossRef - Prevalence of Hyperthyroidism and Hypothyroidism and its Correlation with Serum Antithyroglobulin among patients in Kirkuk-Iraq
Sabah Mohammed Salih, Wijdan Abdullameer Kamel, Mohammed Talat Abbas, Kasim Sakran Abass
Journal Of Advanced Pharmacy Education And Research.2021; 11(2): 57. CrossRef - A nationwide study of patients with monoclonal gammopathy of undetermined significance with a 10-year follow-up in South Korea
Ka-Won Kang, Ji Eun Song, Byung-Hyun Lee, Min Ji Jeon, Eun Sang Yu, Dae Sik Kim, Se Ryeon Lee, Hwa Jung Sung, Chul Won Choi, Yong Park, Byung Soo Kim
Scientific Reports.2021;[Epub] CrossRef - Incidence and Mortality of Myocardial Infarction and Stroke in Patients with Hyperthyroidism: A Nationwide Cohort Study in Korea
Hyun Jung Kim, Taeuk Kang, Min Ji Kang, Hyeong Sik Ahn, Seo Young Sohn
Thyroid.2020; 30(7): 955. CrossRef - Vitamin D supplementation does not prevent the recurrence of Graves’ disease
Yoon Young Cho, Yun Jae Chung
Scientific Reports.2020;[Epub] CrossRef - Binding and Activity of Tetrabromobisphenol A Mono-Ether Structural Analogs to Thyroid Hormone Transport Proteins and Receptors
Xiao-Min Ren, Linlin Yao, Qiao Xue, Jianbo Shi, Qinghua Zhang, Pu Wang, Jianjie Fu, Aiqian Zhang, Guangbo Qu, Guibin Jiang
Environmental Health Perspectives.2020;[Epub] CrossRef - Epidemiology of metabolic syndrome and its components in Chinese patients with a range of thyroid-stimulating hormone concentrations
Kun Tang, Qiao Zhang, Nian-chun Peng, Miao Zhang, Shu-jing Xu, Hong Li, Ying Hu, Chun-ju Xue, Li-xin Shi
Journal of International Medical Research.2020; 48(11): 030006052096687. CrossRef - The Association of Overt and Subclinical Hyperthyroidism with the Risk of Cardiovascular Events and Cardiovascular Mortality: Meta-Analysis and Systematic Review of Cohort Studies
Seo Young Sohn, Eunyoung Lee, Min Kyung Lee, Jae Hyuk Lee
Endocrinology and Metabolism.2020; 35(4): 786. CrossRef - Prevalence of Thyroid Disease in Patients Surgically Treated for Pituitary Disease
Kim, Cho, Ku, Jung, Moon, Kim, Shin, Kim, Lee
Journal of Clinical Medicine.2019; 8(8): 1142. CrossRef - Association of Thyroid-Stimulating Hormone and Thyroid Hormones with Cardiometabolic Risk Factors in Euthyroid Children and Adolescents Aged 10–18 Years: A Population-Based Study
Cheol Gyu Ma, Young Suk Shim
Scientific Reports.2019;[Epub] CrossRef - Weight change is significantly associated with risk of thyroid cancer: A nationwide population-based cohort study
Hyemi Kwon, Kyung-Do Han, Cheol-Young Park
Scientific Reports.2019;[Epub] CrossRef - Evaluation of the relationship of subclinical hypothyroidism with metabolic syndrome and its components in adolescents: a population-based study
Min-Kyung Lee, Yoo Mee Kim, Seo-Young Sohn, Jae-Hyuk Lee, Young Jun Won, Se Hwa Kim
Endocrine.2019; 65(3): 608. CrossRef - Autoimmune thyroiditis and central serous chorioretinopathy may have a relation
Brijesh Takkar, Harsha Saxena, Anubha Rathi, Rekha Singh
Medical Hypotheses.2018; 121: 180. CrossRef
- Diabetes
- Pioglitazone Attenuates Palmitate-Induced Inflammation and Endoplasmic Reticulum Stress in Pancreatic β-Cells
-
Seok-Woo Hong, Jinmi Lee, Jung Hwan Cho, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Cheol-Young Park, Ki-Won Oh, Sung-Woo Park, Won-Young Lee
-
Endocrinol Metab. 2018;33(1):105-113. Published online March 21, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.1.105
-
-
6,289
View
-
96
Download
-
19
Web of Science
-
23
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
The nuclear receptor peroxisome proliferator-activator gamma (PPARγ) is a useful therapeutic target for obesity and diabetes, but its role in protecting β-cell function and viability is unclear. MethodsTo identify the potential functions of PPARγ in β-cells, we treated mouse insulinoma 6 (MIN6) cells with the PPARγ agonist pioglitazone in conditions of lipotoxicity, endoplasmic reticulum (ER) stress, and inflammation. ResultsPalmitate-treated cells incubated with pioglitazone exhibited significant improvements in glucose-stimulated insulin secretion and the repression of apoptosis, as shown by decreased caspase-3 cleavage and poly (adenosine diphosphate [ADP]-ribose) polymerase activity. Pioglitazone also reversed the palmitate-induced expression of inflammatory cytokines (tumor necrosis factor α, interleukin 6 [IL-6], and IL-1β) and ER stress markers (phosphor-eukaryotic translation initiation factor 2α, glucose-regulated protein 78 [GRP78], cleaved-activating transcription factor 6 [ATF6], and C/EBP homologous protein [CHOP]), and pioglitazone significantly attenuated inflammation and ER stress in lipopolysaccharide- or tunicamycin-treated MIN6 cells. The protective effect of pioglitazone was also tested in pancreatic islets from high-fat-fed KK-Ay mice administered 0.02% (wt/wt) pioglitazone or vehicle for 6 weeks. Pioglitazone remarkably reduced the expression of ATF6α, GRP78, and monocyte chemoattractant protein-1, prevented α-cell infiltration into the pancreatic islets, and upregulated glucose transporter 2 (Glut2) expression in β-cells. Moreover, the preservation of β-cells by pioglitazone was accompanied by a significant reduction of blood glucose levels. ConclusionAltogether, these results support the proposal that PPARγ agonists not only suppress insulin resistance, but also prevent β-cell impairment via protection against ER stress and inflammation. The activation of PPARγ might be a new therapeutic approach for improving β-cell survival and insulin secretion in patients with diabetes mellitus
-
Citations
Citations to this article as recorded by  - Nr1h4 and Thrb ameliorate ER stress and provide protection in the MPTP mouse model of Parkinson’s
Nancy Ahuja, Shalini Gupta, Rashmi Arora, Ella Bhagyaraj, Drishti Tiwari, Sumit Kumar, Pawan Gupta
Life Science Alliance.2024; 7(7): e202302416. CrossRef - Prosthetic vascular grafts engineered to combat calcification: Progress and future directions
Taylor K. Brown, Sara Alharbi, Karen J. Ho, Bin Jiang
Biotechnology and Bioengineering.2023; 120(4): 953. CrossRef - Obesity, diabetes mellitus, and cardiometabolic risk: An Obesity Medicine Association (OMA) Clinical Practice Statement (CPS) 2023
Harold Edward Bays, Shagun Bindlish, Tiffany Lowe Clayton
Obesity Pillars.2023; 5: 100056. CrossRef - Metformin promotes osteogenic differentiation and prevents hyperglycaemia-induced osteoporosis by suppressing PPARγ expression
Lifeng Zheng, Ximei Shen, Yun Xie, Hong Lian, Sunjie Yan, Shizhong Wang
Acta Biochimica et Biophysica Sinica.2023; 55(3): 394. CrossRef - Peroxisome proliferator-activated receptors as targets to treat metabolic diseases: Focus on the adipose tissue, liver, and pancreas
Henrique Souza-Tavares, Carolline Santos Miranda, Isabela Macedo Lopes Vasques-Monteiro, Cristian Sandoval, Daiana Araujo Santana-Oliveira, Flavia Maria Silva-Veiga, Aline Fernandes-da-Silva, Vanessa Souza-Mello
World Journal of Gastroenterology.2023; 29(26): 4136. CrossRef - Nicotinamide N-methyltransferase upregulation contributes to palmitate-elicited peroxisome proliferator-activated receptor transactivation in hepatocytes
Qing Song, Jun Wang, Alexandra Griffiths, Samuel Man Lee, Iredia D. Iyamu, Rong Huang, Jose Cordoba-Chacon, Zhenyuan Song
American Journal of Physiology-Cell Physiology.2023; 325(1): C29. CrossRef - The global perspective on peroxisome proliferator-activated receptor γ (PPARγ) in ectopic fat deposition: A review
Yanhao Qiu, Mailin Gan, Xingyu Wang, Tianci Liao, Qiuyang Chen, Yuhang Lei, Lei Chen, Jinyong Wang, Ye Zhao, Lili Niu, Yan Wang, Shunhua Zhang, Li Zhu, Linyuan Shen
International Journal of Biological Macromolecules.2023; 253: 127042. CrossRef - Chemical inducer of regucalcin attenuates lipopolysaccharide‐induced inflammatory responses in pancreatic MIN6 β‐cells and RAW264.7 macrophages
Tomiyasu Murata, Kazunori Hashimoto, Susumu Kohno, Chiaki Takahashi, Masayoshi Yamaguchi, Chihiro Ito, Itoigawa Masataka, Roji Kojima, Kiyomi Hikita, Norio Kaneda
FEBS Open Bio.2022; 12(1): 175. CrossRef - Targets for rescue from fatty acid-induced lipotoxicity in pancreatic beta cells
Seok-Woo Hong, Won-Young Lee
Cardiovascular Prevention and Pharmacotherapy.2022; 4(2): 57. CrossRef - Analysis of changes in the proteomic profile of porcine corpus luteum during different stages of the oestrous cycle: effects of PPAR gamma ligands
Zuzanna Kunicka, Karol Mierzejewski, Aleksandra Kurzyńska, Robert Stryiński, Jesús Mateos, Mónica Carrera, Monika Golubska, Iwona Bogacka, Xiaolong Wang
Reproduction, Fertility and Development.2022; 34(11): 776. CrossRef - Activation of PPARγ Protects Obese Mice from Acute Lung Injury by Inhibiting Endoplasmic Reticulum Stress and Promoting Mitochondrial Biogenesis
Yin Tang, Ke Wei, Ling Liu, Jingyue Ma, Siqi Wu, Wenjing Tang, Stéphane Mandard
PPAR Research.2022; 2022: 1. CrossRef - Effect of Pioglitazone on endoplasmic reticulum stress regarding in situ perfusion rat model
Vivien Telek, Luca Erlitz, Ibitamuno Caleb, Tibor Nagy, Mónika Vecsernyés, Bálint Balogh, György Sétáló, Péter Hardi, Gábor Jancsó, Ildikó Takács
Clinical Hemorheology and Microcirculation.2021; 79(2): 311. CrossRef - Inflammation in Metabolic Diseases and Insulin Resistance
Won-Young Lee
Cardiovascular Prevention and Pharmacotherapy.2021; 3(2): 31. CrossRef - Current Status of Endoplasmic Reticulum Stress in Type II Diabetes
Sagir Mustapha, Mustapha Mohammed, Ahmad Khusairi Azemi, Abubakar Ibrahim Jatau, Aishatu Shehu, Lukman Mustapha, Ibrahim Muazzamu Aliyu, Rabi’u Nuhu Danraka, Abdulbasit Amin, Auwal Adam Bala, Wan Amir Nizam Wan Ahmad, Aida Hanum Ghulam Rasool, Mohd Rais M
Molecules.2021; 26(14): 4362. CrossRef - JunD Regulates Pancreatic β-Cells Function by Altering Lipid Accumulation
Kexin Wang, Yixin Cui, Peng Lin, Zhina Yao, Yu Sun
Frontiers in Endocrinology.2021;[Epub] CrossRef - Pioglitazone even at low dosage improves NAFLD in type 2 diabetes: clinical and pathophysiological insights from a subgroup of the TOSCA.IT randomised trial
Giuseppe Della Pepa, Marco Russo, Marilena Vitale, Fabrizia Carli, Claudia Vetrani, Maria Masulli, Gabriele Riccardi, Olga Vaccaro, Amalia Gastaldelli, Angela A. Rivellese, Lutgarda Bozzetto
Diabetes Research and Clinical Practice.2021; 178: 108984. CrossRef - Radioprotective Effect of Pioglitazone Against Genotoxicity Induced by Ionizing Radiation in Healthy Human Lymphocytes
Roya Kazemi, Seyed J. Hosseinimehr
Cardiovascular & Hematological Agents in Medicinal Chemistry .2021; 19(1): 72. CrossRef - Recent Insights Into Mechanisms of β-Cell Lipo- and Glucolipotoxicity in Type 2 Diabetes
Maria Lytrivi, Anne-Laure Castell, Vincent Poitout, Miriam Cnop
Journal of Molecular Biology.2020; 432(5): 1514. CrossRef - Artemisinin and dihydroartemisinin promote β-cell apoptosis induced by palmitate via enhancing ER stress
Ke Chen, Hu Hua, Ziyang Zhu, Tong Wu, Zhanjun Jia, Qianqi Liu
Apoptosis.2020; 25(3-4): 192. CrossRef - Mechanisms of impaired pancreatic β‑cell function in high‑fat diet‑induced obese mice: The role of endoplasmic reticulum stress
Xiaoqing Yi, Xuan Cai, Sisi Wang, Yanfeng Xiao
Molecular Medicine Reports.2020;[Epub] CrossRef - Docosahexaenoic and Eicosapentaenoic Acids Prevent Altered-Muc2 Secretion Induced by Palmitic Acid by Alleviating Endoplasmic Reticulum Stress in LS174T Goblet Cells
Quentin Escoula, Sandrine Bellenger, Michel Narce, Jérôme Bellenger
Nutrients.2019; 11(9): 2179. CrossRef - PPAR-γ agonist, pioglitazone, reduced oxidative and endoplasmic reticulum stress associated with L-NAME-induced hypertension in rats
Eman Soliman, Shereen F. Behairy, Nabila N. El-maraghy, Shimaa M. Elshazly
Life Sciences.2019; 239: 117047. CrossRef - Changes of MODY signal pathway genes in the endoplasmic reticulum stress in INS-1-3 cells
Yanan Dong, Shirui Li, Wenhui Zhao, Yanlei Wang, Tingting Ge, Jianzhong Xiao, Yukun Li, Herve Le Stunff
PLOS ONE.2018; 13(6): e0198614. CrossRef
- Diabetes
- The Association between Persistent Hypertriglyceridemia and the Risk of Diabetes Development: The Kangbuk Samsung Health Study
-
Yu Hyun Kwon, Seul-Ki Kim, Jung Hwan Cho, Hyemi Kwon, Se Eun Park, Hyung-Geun Oh, Cheol-Young Park, Won-Young Lee, Ki-Won Oh, Sung-Woo Park, Eun-Jung Rhee
-
Endocrinol Metab. 2018;33(1):55-61. Published online January 30, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.1.55
-
-
4,192
View
-
62
Download
-
13
Web of Science
-
14
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Hypertriglyceridemia is known to have an association with increased risks of insulin resistance and diabetes. The aim of this study was to investigate the risk of diabetes mellitus, according to changes in the concentrations of triglycerides, over time. MethodsA total of 15,932 non-diabetic participants (mean age 43.2 years, 68% men) who attended five consecutive annual health check-ups at Kangbuk Samsung Hospital, between January 2010 and December 2014, were recruited. Participants were classified according to their triglyceride concentrations; normal (<150 mg/dL) and abnormal (≥150 mg/dL). According to the triglyceride levels in 2010 and 2012, subjects were divided into four groups: normal-normal, normal-abnormal, abnormal-normal, and abnormal-abnormal. The risk for incident diabetes was assessed in 2014. ResultsAmong the total subjects, 67.5% belonged to the normal-normal group, 8.6% to the normal-abnormal group, 9.4% to the abnormal-normal group, and 14.5% to the abnormal-abnormal group. A total of 234 subjects (1.5%) were newly diagnosed with diabetes, between 2010 and 2014. Over 4 years, 1%, 1.5%, 2.1%, and 3.0% of the subjects developed diabetes in the normal-normal, normal-abnormal, abnormal-normal, and abnormal-abnormal groups, respectively. When the risk for incident diabetes was analyzed in the groups, after adjusting the confounding variables, a 1.58-fold increase in the risk of diabetes (95% confidence interval [CI], 1.10 to 2.26) was observed in the participants with persistent hypertriglyceridemia (abnormal-abnormal group). This was attenuated by further adjustments for body mass index (BMI) (hazard ratio, 1.25; 95% CI, 0.86 to 1.80). ConclusionIn this large study population, persistent hypertriglyceridemia, over a period of 2 years, was significantly associated with the risk of incident diabetes, which was attenuated after adjustment for BMI.
-
Citations
Citations to this article as recorded by  - Cumulative exposure to hypertriglyceridemia and risk of type 2 diabetes in young adults
Min-Kyung Lee, Kyungdo Han, Bongsung Kim, Jong-Dai Kim, Moon Jung Kim, Byungpyo Kim, Jung Heo, Jiyeon Ahn, Seo-Young Sohn, Jae-Hyuk Lee
Diabetes Research and Clinical Practice.2024; 208: 111109. CrossRef - Usefulness of SPISE Index for Screening and Detection of Early Stages of Insulin Resistance among Chilean Young Adults
Isabel Pereyra González, Sandra Lopez-Arana
Annals of Nutrition and Metabolism.2023; 79(4): 372. CrossRef - Lipid variability in patients with diabetes mellitus
Jeongmin Lee, Seung-Hwan Lee
Cardiovascular Prevention and Pharmacotherapy.2023; 5(4): 126. CrossRef - Sesamin: A Promising Therapeutic Agent for Ameliorating Symptoms of Diabetes
Shu-Ming Huang, Cheng-Hung Chuang, Christine Joyce F. Rejano, Lemmuel L. Tayo, Cheng-Yang Hsieh, Steven Kuan-Hua Huang, Po-Wei Tsai
Molecules.2023; 28(21): 7255. CrossRef - Variability, Mean, and Baseline Values of Metabolic Parameters in Predicting Risk of Type 2 Diabetes
Duong Duc Pham, Jaekyung Song, Yunwan Jeon, Ibrahimi Hajar, Chae Hun Leem
The Journal of Clinical Endocrinology & Metabolism.2022; 107(5): 1270. CrossRef - Lipid Variability and Diabetes Mellitus
Jeongmin Lee, Seung-Hwan Lee
The Journal of Korean Diabetes.2022; 23(1): 28. CrossRef - The Risk of Type 2 Diabetes Mellitus in a Russian Population Cohort According to Data from the HAPIEE Project
Svetlana V. Mustafina, Oksana D. Rymar, Liliya V. Shcherbakova, Evgeniy G. Verevkin, Hynek Pikhart, Olga V. Sazonova, Yuliya I. Ragino, Galina I. Simonova, Martin Bobak, Sofia K. Malyutina, Mikhail I. Voevoda
Journal of Personalized Medicine.2021; 11(2): 119. CrossRef - The influence of VDR polymorphisms on the type 2 diabetes susceptibility in Chinese: an interaction with hypertriglyceridemia
Dongdong Zhang, Cheng Cheng, Yan Wang, Yuan Xue, Yaping Liu, Yiming Liu, Mingming Feng, Ze Xu, Wenjie Li, Xing Li
Molecular Genetics and Genomics.2021; 296(4): 837. CrossRef - Development and validation of a new diabetes index for the risk classification of present and new-onset diabetes: multicohort study
Shinje Moon, Ji-Yong Jang, Yumin Kim, Chang-Myung Oh
Scientific Reports.2021;[Epub] CrossRef - Hypertriglyceridemia as an Independent Predictor for Ten-Year Incidence of Diabetes in Thais
Suranut Charoensri, Supatida Turnsaket, Chatlert Pongchaiyakul
Vascular Health and Risk Management.2021; Volume 17: 519. CrossRef - Prevalence and Current Management of Cardiovascular Risk Factors in Korean Adults Based on Fact Sheets
Eun-Jung Rhee
Endocrinology and Metabolism.2020; 35(1): 85. CrossRef - HDL-Cholesterol, Its Variability, and the Risk of Diabetes: A Nationwide Population-Based Study
Seung-Hwan Lee, Hun-Sung Kim, Yong-Moon Park, Hyuk-Sang Kwon, Kun-Ho Yoon, Kyungdo Han, Mee Kyoung Kim
The Journal of Clinical Endocrinology & Metabolism.2019; 104(11): 5633. CrossRef - Response: The Association between Persistent Hypertriglyceridemia and the Risk of Diabetes Development: The Kangbuk Samsung Health Study (Endocrinol Metab 2018;33:55–61, Yu Hyun Kwon et al.)
Eun-Jung Rhee, Yu Hyun Kwon
Endocrinology and Metabolism.2018; 33(3): 425. CrossRef - The Association between Persistent Hypertriglyceridemia and the Risk of Diabetes Development: The Kangbuk Samsung Health Study (Endocrinol Metab 2018;33:55–61, Yu Hyun Kwon et al.)
Mi Hae Seo
Endocrinology and Metabolism.2018; 33(2): 305. CrossRef
- Thyroid
- Comparison of Immunohistochemistry and Direct Sanger Sequencing for Detection of the BRAFV600E Mutation in Thyroid Neoplasm
-
Hye-Seon Oh, Hyemi Kwon, Suyeon Park, Mijin Kim, Min Ji Jeon, Tae Yong Kim, Young Kee Shong, Won Bae Kim, Jene Choi, Won Gu Kim, Dong Eun Song
-
Endocrinol Metab. 2018;33(1):62-69. Published online January 30, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.1.62
-
-
5,837
View
-
69
Download
-
17
Web of Science
-
19
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
The BRAFV600E mutation is the most common genetic alteration identified in papillary thyroid carcinoma (PTC). Because of its costs effectiveness and sensitivity, direct Sanger sequencing has several limitations. The aim of this study was to evaluate the efficiency of immunohistochemistry (IHC) as an alternative method to detect the BRAFV600E mutation in preoperative and postoperative tissue samples. MethodsWe evaluated 71 patients who underwent thyroid surgery with the result of direct sequencing of the BRAFV600E mutation. IHC staining of the BRAFV600E mutation was performed in 49 preoperative and 23 postoperative thyroid specimens. ResultsSixty-two patients (87.3%) had PTC, and of these, BRAFV600E was confirmed by direct sequencing in 57 patients (91.9%). In 23 postoperative tissue samples, the BRAFV600E mutation was detected in 16 samples (70%) by direct sequencing and 18 samples (78%) by IHC. In 24 fine needle aspiration (FNA) samples, BRAFV600E was detected in 18 samples (75%) by direct sequencing and 16 samples (67%) by IHC. In 25 core needle biopsy (CNB) samples, the BRAFV600E mutation was detected in 15 samples (60%) by direct sequencing and 16 samples (64%) by IHC. The sensitivity and specificity of IHC for detecting the BRAFV600E mutation were 77.8% and 66.7% in FNA samples and 99.3% and 80.0% in CNB samples. ConclusionIHC could be an alternative method to direct Sanger sequencing for BRAFV600E mutation detection both in postoperative and preoperative samples. However, application of IHC to detect the BRAFV600E mutation in FNA samples is of limited value compared with direct sequencing.
-
Citations
Citations to this article as recorded by  - Circulating Nucleic Acids in Colorectal Cancer: Diagnostic and Prognostic Value
Somayeh Igder, Mozhdeh Zamani, Shima Fakher, Morvarid Siri, Hassan Ashktorab, Negar Azarpira, Pooneh Mokarram, Sowjanya Thatikonda
Disease Markers.2024; 2024: 1. CrossRef - The Accurate Interpretation and Clinical Significance of Morphological Features of Fine Needle Aspiration Cells in Papillary Thyroid Carcinoma
Xue-Jiao Xiong, Ming-Ming Xiao, Yi-Xia Zhang, Dong-Ge Liu, Mu-Lan Jin, Jian Wang, Hong-Tao Xu, Qing-Chang Li, Guang-Ping Wu, Giovanni Tuccari
Analytical Cellular Pathology.2023; 2023: 1. CrossRef - An effective approach for BRAF V600E mutation analysis of routine thyroid fine needle aspirates
Tanupriya Agrawal, Liqiang Xi, Winnifred Navarro, Mark Raffeld, Snehal B. Patel, Mark J. Roth, Joanna Klubo‐Gwiezdzinska, Armando C. Filie
Cytopathology.2022; 33(3): 344. CrossRef - A dual identification strategy based on padlock ligation and CRISPR/Cas14a for highly specific detection of BRAF V600E mutation in clinical samples
Weicheng Shi, Yao Gong, Decai Zhang, Tiantian Yang, Ming Yi, Jingyi Tan, Shijia Ding, Wei Cheng
Analytical Methods.2022; 14(19): 1913. CrossRef - Research Progress of BRAF V600E Gene Mutation in Papillary Thyroid Carcinoma
延泽 刘
Advances in Clinical Medicine.2022; 12(09): 8499. CrossRef - VE1 immunohistochemistry is an adjunct tool for detection of BRAFV600E mutation: Validation in thyroid cancer patients
Faiza A. Rashid, Sobia Tabassum, Mosin S. Khan, Hifzur R. Ansari, Muhammad Asif, Ahmareen K. Sheikh, Syed Sameer Aga
Journal of Clinical Laboratory Analysis.2021;[Epub] CrossRef - BRAF testing in a South African cohort of MLH1 deficient endometrial carcinomas: lessons learnt
Reubina Wadee, Wayne Grayson
Southern African Journal of Gynaecological Oncology.2021; 13(1): 1. CrossRef - Association between mutation profiles and clinicopathological features in Chinese patients with thyroid cancer
Changwen Jing, Haixia Cao, Rong Ma, Jianzhong Wu, Zhuo Wang
Precision Medical Sciences.2021; 10(3): 113. CrossRef - Development of a Molecular Assay for Detection and Quantification of theBRAFVariation in Residual Tissue From Thyroid Nodule Fine-Needle Aspiration Biopsy Specimens
Guodong Fu, Ronald S. Chazen, Christina MacMillan, Ian J. Witterick
JAMA Network Open.2021; 4(10): e2127243. CrossRef - Variations in MAP kinase gladiators and risk of differentiated thyroid carcinoma
Faiza Rashid, Ghulam Bhat, Mosin Khan, Sobia Tabassum, Mohammad Bhat
Molecular and Clinical Oncology.2021;[Epub] CrossRef - Порівняльне імуногістохімічне дослідження BRAFV600E-позитивних і BRAFV600E-негативних радіогенних і спорадичних папілярних тиреоїдних карцином
L. Yu. Zurnadzhy, T.I. Rogounovitch, V.O. Saenko, M.Yu. Bolgov, S.V. Masiuk, S.V. Burko, T.L. Degtyaryova, S.V. Chernyshov, S.V. Gulevatyi, N. Mitsutake, M.D. Tronko, T.I. Bogdanova
Endokrynologia.2021; 26(2): 105. CrossRef - Evaluation of the expression levels of BRAFV600E mRNA in primary tumors of thyroid cancer using an ultrasensitive mutation assay
Tien Viet Tran, Kien Xuan Dang, Quynh Huong Pham, Ung Dinh Nguyen, Nhung Thi Trang Trinh, Luong Van Hoang, Son Anh Ho, Ba Van Nguyen, Duc Trong Nguyen, Dung Tuan Trinh, Dung Ngoc Tran, Arto Orpana, Ulf-Håkan Stenman, Jakob Stenman, Tho Huu Ho
BMC Cancer.2020;[Epub] CrossRef - VE1 Immunohistochemistry Improves the Limit of Genotyping for Detecting BRAFV600E Mutation in Papillary Thyroid Cancer
Sonam Choden, Somboon Keelawat, Chan Kwon Jung, Andrey Bychkov
Cancers.2020; 12(3): 596. CrossRef - Comparison of Molecular Methods and BRAF Immunohistochemistry (VE1 Clone) for the Detection of BRAF V600E Mutation in Papillary Thyroid Carcinoma: A Meta-Analysis
Kyle G. Parker, Michael G. White, Nicole A. Cipriani
Head and Neck Pathology.2020; 14(4): 1067. CrossRef - Next generation sequencing based detection of 15 target genes mutations in papillary thyroid carcinoma
Zhuo Wang, Changwen Jing, Haixia Cao, SiWen Liu, Jianzhong Wu, Rong Ma
Precision Medical Sciences.2020; 9(2): 90. CrossRef - A Systematic Review and Meta-Analysis of the Diagnostic Performance of BRAF V600E Immunohistochemistry in Thyroid Histopathology
Ranjit Singarayer, Ozgur Mete, Laure Perrier, Lehana Thabane, Sylvia L. Asa, Stan Van Uum, Shereen Ezzat, David P. Goldstein, Anna M. Sawka
Endocrine Pathology.2019; 30(3): 201. CrossRef - Comparison of droplet digital PCR and direct Sanger sequencing for the detection of the BRAFV600E mutation in papillary thyroid carcinoma
Zhuo Wang, Kejing Sun, Changwen Jing, Haixia Cao, Rong Ma, Jianzhong Wu
Journal of Clinical Laboratory Analysis.2019;[Epub] CrossRef - Immunohistochemistry Innovations for Diagnosis and Tissue-Based Biomarker Detection
Narittee Sukswai, Joseph D. Khoury
Current Hematologic Malignancy Reports.2019; 14(5): 368. CrossRef - Immunohistochemistry is a feasible method to screen BRAF V600E mutation in colorectal and papillary thyroid carcinoma
Xiangyan Zhang, Lili Wang, Jigang Wang, Han Zhao, Jie Wu, Shuhong Liu, Lu Zhang, Yujun Li, Xiaoming Xing
Experimental and Molecular Pathology.2018; 105(1): 153. CrossRef
- Clinical Study
- Molecular Diagnosis Using Residual Liquid-Based Cytology Materials for Patients with Nondiagnostic or Indeterminate Thyroid Nodules
-
Hyemi Kwon, Won Gu Kim, Markus Eszlinger, Ralf Paschke, Dong Eun Song, Mijin Kim, Suyeon Park, Min Ji Jeon, Tae Yong Kim, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2016;31(4):586-591. Published online November 4, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.4.586
-
-
4,202
View
-
42
Download
-
11
Web of Science
-
12
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Molecular analysis for common somatic mutations in thyroid cancer can improve diagnostic accuracy of fine-needle aspiration cytology (FNAC) in the nondiagnostic or indeterminate category of thyroid nodules. In this study, we evaluated the feasibility of molecular diagnosis from residual liquid-based cytology (LBC) material after cytological diagnosis. MethodsThis prospective study enrolled 53 patients with thyroid nodules diagnosed as nondiagnostic, atypia of undetermined significance (AUS), or follicular lesion of undetermined significance (FLUS) after FNAC. DNAs and RNAs were isolated from residual LBC materials. BRAFV600E and RAS point mutations, PAX8/peroxisome proliferator-activated receptor γ (PPARγ), RET/PTC1, and RET/PTC3 rearrangements were evaluated by real-time polymerase chain reaction and pyrosequencing. ResultsAll DNAs from 53 residual LBC samples could be analysed and point mutations were detected in 10 samples (19%). In 17 AUS nodules, seven samples (41%) had point mutations including BRAF (n=4), NRAS (n=2), and KRAS (n=1). In 20 FLUS nodules, three samples (15%) had NRAS point mutations. RNA from only one FLUS nodule could be analysed for rearrangements and there was no abnormality. ConclusionMolecular analysis for BRAF and RAS mutations was feasible in residual LBC materials and might be useful for diagnosis of indeterminate thyroid nodules.
-
Citations
Citations to this article as recorded by  - Kras Gene Analysis Using Liquid-Based Cytology Specimens Predicts Therapeutic Responses and Prognosis in Patients with Pancreatic Cancer
Masahiro Itonaga, Reiko Ashida, Shin-Ichi Murata, Yasunobu Yamashita, Keiichi Hatamaru, Takashi Tamura, Yuki Kawaji, Yuudai Kayama, Tomoya Emori, Manabu Kawai, Hiroki Yamaue, Ibu Matsuzaki, Hirokazu Nagai, Yuichi Kinoshita, Ke Wan, Toshio Shimokawa, Masay
Cancers.2022; 14(3): 551. CrossRef - From Traditional Histology to Next-Generation Pathology: A Review of The Workflow for the Characterisation and Molecular Profiling of Non-Small Cell Lung Cancer Samples
EMJ Oncology.2020;[Epub] CrossRef - Preanalytic variables in quality and quantity of nucleic acids extracted from FNA specimens of thyroid gland nodules collected in CytoLyt: Cellularity and storage time
Jonas J. Heymann, Lorene M. Yoxtheimer, Hyeon Jin Park, Evan M. Fernandez, Kirk E. Facey, Susan A. Alperstein, Hung V. Tran, Inji Baek, Theresa Scognamiglio, Hanna Rennert, Momin T. Siddiqui, Wei Song
Cancer Cytopathology.2020; 128(9): 656. CrossRef - Diagnostic accuracy of molecular testing with three molecular markers on thyroid fine‐needle aspiration cytology with abnormal category
Hatice Seneldir, Gozde Kir, Tuce Soylemez, Rabia B. Girgin, Nurver Ozbay, Filiz Ozen, Handan Ankarali, Gurhan Bas, Orhan Alimoglu
Diagnostic Cytopathology.2020; 48(6): 507. CrossRef - Small but powerful: the promising role of small specimens for biomarker testing
Qiong Gan, Sinchita Roy-Chowdhuri
Journal of the American Society of Cytopathology.2020; 9(5): 450. CrossRef - Centrifuged supernatants from FNA provide a liquid biopsy option for clinical next‐generation sequencing of thyroid nodules
Wenrui Ye, Brette Hannigan, Stephanie Zalles, Meenakshi Mehrotra, Bedia A. Barkoh, Michelle D. Williams, Maria E. Cabanillas, Beth Edeiken‐Monroe, Peter Hu, Dzifa Duose, Ignacio I. Wistuba, L. Jeffrey Medeiros, John Stewart, Rajyalakshmi Luthra, Sinchita
Cancer Cytopathology.2019; 127(3): 146. CrossRef - Molecular testing of residual cytology samples: Rethink, reclaim, repurpose
Sinchita Roy‐Chowdhuri
Cancer Cytopathology.2019; 127(1): 15. CrossRef - K-ras mutation analysis of residual liquid-based cytology specimens from endoscopic ultrasound-guided fine needle aspiration improves cell block diagnosis of pancreatic ductal adenocarcinoma
Yoko Sekita-Hatakeyama, Takeshi Nishikawa, Mao Takeuchi, Kouhei Morita, Maiko Takeda, Kinta Hatakeyama, Tokiko Nakai, Tomoko Uchiyama, Hiroe Itami, Tomomi Fujii, Akira Mitoro, Masayuki Sho, Chiho Ohbayashi, Giancarlo Troncone
PLOS ONE.2018; 13(3): e0193692. CrossRef - Comparison of Immunohistochemistry and Direct Sanger Sequencing for Detection of theBRAFV600EMutation in Thyroid Neoplasm
Hye-Seon Oh, Hyemi Kwon, Suyeon Park, Mijin Kim, Min Ji Jeon, Tae Yong Kim, Young Kee Shong, Won Bae Kim, Jene Choi, Won Gu Kim, Dong Eun Song
Endocrinology and Metabolism.2018; 33(1): 62. CrossRef - Next-Generation Sequencing Identifies Gene Mutations That Are Predictive of Malignancy in Residual Needle Rinses Collected From Fine-Needle Aspirations of Thyroid Nodules
Maren Y. Fuller, Dina Mody, April Hull, Kristi Pepper, Heather Hendrickson, Randall Olsen
Archives of Pathology & Laboratory Medicine.2018; 142(2): 178. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Loss of c-KIT expression in thyroid cancer cells
Sara Franceschi, Francesca Lessi, Federica Panebianco, Elena Tantillo, Marco La Ferla, Michele Menicagli, Paolo Aretini, Alessandro Apollo, Antonio Giuseppe Naccarato, Ivo Marchetti, Chiara Maria Mazzanti, Aamir Ahmad
PLOS ONE.2017; 12(3): e0173913. CrossRef
- Clinical Study
- Usefulness of Measuring Thyroid Stimulating Antibody at the Time of Antithyroid Drug Withdrawal for Predicting Relapse of Graves Disease
-
Hyemi Kwon, Won Gu Kim, Eun Kyung Jang, Mijin Kim, Suyeon Park, Min Ji Jeon, Tae Yong Kim, Jin-Sook Ryu, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2016;31(2):300-310. Published online April 25, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.2.300
-
-
5,004
View
-
87
Download
-
20
Web of Science
-
19
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Hyperthyroidism relapse in Graves disease after antithyroid drug (ATD) withdrawal is common; however, measuring the thyrotropin receptor antibody (TRAb) at ATD withdrawal in order to predict outcomes is controversial. This study compared measurement of thyroid stimulatory antibody (TSAb) and thyrotropin-binding inhibitory immunoglobulin (TBII) at ATD withdrawal to predict relapse. MethodsThis retrospective study enrolled patients with Graves disease who were treated with ATDs and whose serum thyroid-stimulating hormone levels were normal after receiving low-dose ATDs. ATD therapy was stopped irrespective of TRAb positivity after an additional 6 months of receiving the minimum dose of ATD therapy. Patients were followed using thyroid function tests and TSAb (TSAb group; n=35) or TBII (TBII group; n=39) every 3 to 6 months for 2 years after ATD withdrawal. ResultsTwenty-eight patients (38%) relapsed for a median follow-up of 21 months, and there were no differences in baseline clinical characteristics between groups. In the TSAb group, relapse was more common in patients with positive TSAb at ATD withdrawal (67%) than patients with negative TSAb (17%; P=0.007). Relapse-free survival was shorter in TSAb-positive patients. In the TBII group, there were no differences in the relapse rate and relapse-free survivals according to TBII positivity. For predicting Graves disease relapse, the sensitivity and specificity of TSAb were 63% and 83%, respectively, whereas those of TBII were 28% and 65%. ConclusionTSAb at ATD withdrawal can predict the relapse of Graves hyperthyroidism, but TBII cannot. Measuring TSAb at ATD withdrawal can assist with clinical decisions making for patients with Graves disease.
-
Citations
Citations to this article as recorded by  - Analysis of Related Factors in Refractory Graves’ Disease
鑫 王
Advances in Clinical Medicine.2023; 13(08): 13439. CrossRef - Interpretation of Thyroid Autoantibodies in Hyperthyroidism
Han-Sang Baek, Dong-Jun Lim
The Korean Journal of Medicine.2023; 98(3): 132. CrossRef - The Early Changes in Thyroid-Stimulating Immunoglobulin Bioassay over Anti-Thyroid Drug Treatment Could Predict Prognosis of Graves’ Disease
Jin Yu, Han-Sang Baek, Chaiho Jeong, Kwanhoon Jo, Jeongmin Lee, Jeonghoon Ha, Min Hee Kim, Jungmin Lee, Dong-Jun Lim
Endocrinology and Metabolism.2023; 38(3): 338. CrossRef - Thyroid-Stimulatory Antibody as a Predictive Factor for Graves’ Disease Relapse
Tiago Da Silva Santos, José Carlos Oliveira, Cláudia Freitas, André Couto de Carvalho
Cureus.2022;[Epub] CrossRef - The Prediction Model Using Thyroid-stimulating Immunoglobulin Bioassay For Relapse of Graves’ Disease
Han-Sang Baek, Jaejun Lee, Chai-Ho Jeong, Jeongmin Lee, Jeonghoon Ha, Kwanhoon Jo, Min-Hee Kim, Jae Hyoung Cho, Moo Il Kang, Dong-Jun Lim
Journal of the Endocrine Society.2022;[Epub] CrossRef - Identification of patients with Graves’ disease who benefit from high-dose radioactive iodine therapy
Shiro Watanabe, Shozo Okamoto, Kazumasa Akikawa, Noriyuki Miyamoto, Miyuki Okamura-Kawasaki, Yuko Uchiyama, Junki Takenaka, Takuya Toyonaga, Kenji Hirata, Kohsuke Kudo
Annals of Nuclear Medicine.2022; 36(11): 923. CrossRef - The relationship between atherosclerotic disease and relapse during ATD treatment
Xinxin Zhu, Yaguang Zhang, Xiaoyu Zhao, Xiaona Zhang, Zixuan Ru, Yanmeizhi Wu, Xu Yang, Boyu Hou, Hong Qiao
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Antithyroid Drug Treatment in Graves’ Disease
Jae Hoon Chung
Endocrinology and Metabolism.2021; 36(3): 491. CrossRef - The prognostic value of thyroid-stimulating immunoglobulin in the management of Graves’ disease
Yulin Zhou, Mengxi Zhou, Yicheng Qi, Weiqing Wang, Xinxin Chen, Shu Wang
Therapeutic Advances in Endocrinology and Metabolism.2021; 12: 204201882110449. CrossRef - Changes in Thyroid Peroxidase and Thyroglobulin Antibodies Might Be Associated with Graves' Disease Relapse after Antithyroid Drug Therapy
Yun Mi Choi, Mi Kyung Kwak, Sang Mo Hong, Eun-Gyoung Hong
Endocrinology and Metabolism.2019; 34(3): 268. CrossRef - Graves' Disease: Can It Be Cured?
Wilmar M. Wiersinga
Endocrinology and Metabolism.2019; 34(1): 29. CrossRef - Medical Treatment of Graves' Disease
Hyun-Kyung Chung
International Journal of Thyroidology.2019; 12(2): 79. CrossRef - When should antithyroid drug therapy to reduce the relapse rate of hyperthyroidism in Graves’ disease be discontinued?
Suyeon Park, Eyun Song, Hye-Seon Oh, Mijin Kim, Min Ji Jeon, Won Gu Kim, Tae Yong Kim, Young Kee Shong, Doo Man Kim, Won Bae Kim
Endocrine.2019; 65(2): 348. CrossRef - Elevated Serum IL-17 Expression at Cessation Associated with Graves’ Disease Relapse
Jianhui Li, Xiaohua Sun, Danzhen Yao, Jinying Xia
International Journal of Endocrinology.2018; 2018: 1. CrossRef - Active Surveillance for Patients With Papillary Thyroid Microcarcinoma: A Single Center’s Experience in Korea
Hyemi Kwon, Hye-Seon Oh, Mijin Kim, Suyeon Park, Min Ji Jeon, Won Gu Kim, Won Bae Kim, Young Kee Shong, Dong Eun Song, Jung Hwan Baek, Ki-Wook Chung, Tae Yong Kim
The Journal of Clinical Endocrinology & Metabolism.2017; 102(6): 1917. CrossRef - Free Thyroxine, Anti-Thyroid Stimulating Hormone Receptor Antibody Titers, and Absence of Goiter Were Associated with Responsiveness to Methimazole in Patients with New Onset Graves' Disease
Hoon Sung Choi, Won Sang Yoo
Endocrinology and Metabolism.2017; 32(2): 281. CrossRef - The Second Antithyroid Drug Treatment Is Effective in Relapsed Graves' Disease Patients: A Median 11-Year Follow-Up Study
Ye An Kim, Sun Wook Cho, Hoon Sung Choi, Shinje Moon, Jae Hoon Moon, Kyung Won Kim, Do Joon Park, Ka Hee Yi, Young Joo Park, Bo Youn Cho
Thyroid.2017; 27(4): 491. CrossRef - The Recurrence Rate of Graves' Disease among Patients with Subclinical Thyrotoxicosis after Initial Remission with Antithyroid Agents
Myoung Sook Shim, Soo Min Nam, Jin Sae Yoo, Hae Kyung Kim, Sang Jun Lee, Mi Young Lee
International Journal of Thyroidology.2017; 10(2): 77. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef
- Clinical Study
- Low Prevalence of Somatic TERT Promoter Mutations in Classic Papillary Thyroid Carcinoma
-
Min Ji Jeon, Won Gu Kim, Soyoung Sim, Seonhee Lim, Hyemi Kwon, Tae Yong Kim, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2016;31(1):100-104. Published online March 16, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.1.100
-
-
4,361
View
-
32
Download
-
16
Web of Science
-
15
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Transcriptional activating mutations of telomerase reverse transcriptase (TERT) are associated with more aggressive thyroid cancer. We evaluated the significance of TERT promoter mutations in Korean patients with classic papillary thyroid cancer (PTC). MethodsGenomic DNA was isolated from four thyroid cancer cell lines and 35 fresh-frozen PTC tissues. TERT promoter mutations (C228T and C250T) and the BRAF V600E mutation were evaluated by polymerase chain reaction amplification and direct sequencing. ResultsThe CC228229TT mutation in the TERT promoter was detected in BCPAP cells and the C250T mutation was found in 8505C cells. No TERT promoter mutation was observed in Cal-62 or ML-1 cells. The C228T mutation was found in only 1 of 35 (2.8%) PTCs and no C250T mutations were detected in any of the study subjects. The BRAF V600E mutation was found in 20 of 35 (57.1%) PTCs. One patient with the C228T TERT mutation also harbored the BRAF V600E mutation and developed a recurrence. ConclusionThe prevalence of somatic TERT promoter mutations was low in Korean patients with classic PTC. Therefore, the prognostic role of TERT promoter mutations might be limited in this patient cohort.
-
Citations
Citations to this article as recorded by  - Risk Factors for TERT Promoter Mutations with Papillary Thyroid Carcinoma Patients: A Meta-Analysis and Systematic Review
Jingxin Mao, Xingliang Huang, Mohammad K. Okla, Mostafa A. Abdel-Maksoud, Ayman Mubarak, Zahid Hameed, Razia Noreen, Aqsa Chaudhary, Shakira Ghazanfar, Yixuan Liao, Yasir Hameed, Chen Li, Min Tang
Computational and Mathematical Methods in Medicine.2022; 2022: 1. CrossRef - Telomerase reverse transcriptase promoter mutations in cancers derived from multiple organ sites among middle eastern population
Abdul K. Siraj, Rong Bu, Kaleem Iqbal, Sandeep Kumar Parvathareddy, Nabil Siraj, Sarah Siraj, Mark Ranier F. Diaz, Dionne Rae Rala, Allianah D. Benito, Maria Angelita Sabido, Maha Al-Rasheed, Khadija A.S. Al-Obaisi, Wael Al-Haqawi, Ingrid G. Victoria, Waf
Genomics.2020; 112(2): 1746. CrossRef - Association between TERT promoter mutations and clinical behaviors in differentiated thyroid carcinoma: a systematic review and meta-analysis
Jing Yang, Yanping Gong, Shuping Yan, Hui Chen, Siqin Qin, Rixiang Gong
Endocrine.2020; 67(1): 44. CrossRef - The Combination of RET, BRAF and Demographic Data Identifies Subsets of Patients with Aggressive Papillary Thyroid Cancer
Jose R. W. Martínez, Sergio Vargas-Salas, Soledad Urra Gamboa, Estefanía Muñoz, José Miguel Domínguez, Augusto León, Nicolás Droppelmann, Antonieta Solar, Mark Zafereo, F. Christopher Holsinger, Hernán E. González
Hormones and Cancer.2019; 10(2-3): 97. CrossRef - Correlation between TERT C228T and clinic-pathological features in pediatric papillary thyroid carcinoma
Jiangqiao Geng, Yuanhu Liu, Yongli Guo, Huanmin Wang, Jun Tai, Yaqiong Jin, Jie Zhang, Yongbo Yu, Shengcai Wang, Yingluan Song, Xin Ni
Science China Life Sciences.2019; 62(12): 1563. CrossRef - Human telomerase reverse transcriptase in papillary thyroid cancer: gene expression, effects of silencing and regulation by BET inhibitors in thyroid cancer cells
Valentina Maggisano, Marilena Celano, Saverio Massimo Lepore, Marialuisa Sponziello, Francesca Rosignolo, Valeria Pecce, Antonella Verrienti, Federica Baldan, Catia Mio, Lorenzo Allegri, Marianna Maranghi, Rosa Falcone, Giuseppe Damante, Diego Russo, Stef
Endocrine.2019; 63(3): 545. CrossRef - BRAF and RAS Mutational Status in Noninvasive Follicular Thyroid Neoplasm with Papillary-Like Nuclear Features and Invasive Subtype of Encapsulated Follicular Variant of Papillary Thyroid Carcinoma in Korea
Mijin Kim, Min Ji Jeon, Hye-Seon Oh, Suyeon Park, Tae Yong Kim, Young Kee Shong, Won Bae Kim, Kyunggon Kim, Won Gu Kim, Dong Eun Song
Thyroid.2018; 28(4): 504. CrossRef - The role of TERT promoter mutations in postoperative and preoperative diagnosis and prognosis in thyroid cancer
Anqi Jin, Jianhao Xu, Yan Wang
Medicine.2018; 97(29): e11548. CrossRef - Telomere Maintenance Mechanisms in Cancer
Tiago Bordeira Gaspar, Ana Sá, José Manuel Lopes, Manuel Sobrinho-Simões, Paula Soares, João Vinagre
Genes.2018; 9(5): 241. CrossRef - Anti-hTERT siRNA-Loaded Nanoparticles Block the Growth of Anaplastic Thyroid Cancer Xenograft
Giovanni E. Lombardo, Valentina Maggisano, Marilena Celano, Donato Cosco, Chiara Mignogna, Federica Baldan, Saverio M. Lepore, Lorenzo Allegri, Sonia Moretti, Cosimo Durante, Giuseppe Damante, Massimo Fresta, Diego Russo, Stefania Bulotta, Efisio Puxeddu
Molecular Cancer Therapeutics.2018; 17(6): 1187. CrossRef - Silencing of hTERT blocks growth and migration of anaplastic thyroid cancer cells
Valentina Maggisano, Marilena Celano, Giovanni Enrico Lombardo, Saverio Massimo Lepore, Marialuisa Sponziello, Francesca Rosignolo, Antonella Verrienti, Federica Baldan, Efisio Puxeddu, Cosimo Durante, Sebastiano Filetti, Giuseppe Damante, Diego Russo, St
Molecular and Cellular Endocrinology.2017; 448: 34. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Telomerase: The Devil Inside
Mukesh Kumar, Andre Lechel, Çagatay Güneş
Genes.2016; 7(8): 43. CrossRef - Cancer-Specific Telomerase Reverse Transcriptase (TERT) Promoter Mutations: Biological and Clinical Implications
Tiantian Liu, Xiaotian Yuan, Dawei Xu
Genes.2016; 7(7): 38. CrossRef - Transcription Regulation of the Human Telomerase Reverse Transcriptase (hTERT) Gene
Muhammad Ramlee, Jing Wang, Wei Toh, Shang Li
Genes.2016; 7(8): 50. CrossRef
- Clinical Study
- Thyrotoxic Periodic Paralysis and Polymorphisms of the ADRB2, AR, and GABRA3 Genes in Men with Graves Disease
-
Suyeon Park, Tae Yong Kim, Soyoung Sim, Seonhee Lim, Mijin Kim, Hyemi Kwon, Min Ji Jeon, Won Gu Kim, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2016;31(1):142-146. Published online March 16, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.1.142
-
-
3,758
View
-
39
Download
-
4
Web of Science
-
4
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Thyrotoxic periodic paralysis (TPP) is a rare complication of thyrotoxicosis characterized by acute attacks of muscle weakness and hypokalemia. Recently, variation in several genes was suggested to be associated with TPP. This study evaluated the genetic predisposition to TPP in terms of the β2-adrenergic receptor (ADRB2), androgen receptor (AR), and γ-aminobutyric acid receptor α3 subunit (GABRA3) genes. MethodsThis study enrolled 48 men with Graves disease (GD) and TPP, and 48 GD patients without TPP. We compared the frequencies of candidate polymorphisms between the two groups. ResultsThe frequency of the Gly16/Gly16 genotype in ADRB2 was not significantly associated with TPP (P=0.32). More CAG repeats (≥26) in the AR gene were not correlated with TPP (odds ratio [OR], 2.46; 95% confidence interval [CI], 0.81 to 8.09; P=0.08). The allele frequency of the TT genotype in the GABRA3 gene was not associated with TPP (OR, 1.83; 95% CI, 0.54 to 6.74; P=0.41). ConclusionThe polymorphisms in the ADRB2, AR, and GABRA3 genes could not explain the genetic susceptibility to TPP in Korean men with GD.
-
Citations
Citations to this article as recorded by  - RNASET2,GPR174, and PTPN22 gene polymorphisms are related to the risk of liver damage associated with the hyperthyroidism in patients with Graves’ disease
Qing Zhang, Shaozheng Liu, Yanxing Guan, Qingjie Chen, Qing Zhang, Xiang Min
Journal of Clinical Laboratory Analysis.2018;[Epub] CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Periodic Paralysis and Encephalopathy as Initial Manifestations of Graves’ Disease
Theocharis Tsironis, Athanasios Tychalas, Dimitrios Kiourtidis, Jannis Kountouras, Georgia Xiromerisiou, Jobst Rudolf, Georgia Deretzi
The Neurologist.2017; 22(4): 134. CrossRef - Thyrotoxic periodic paralysis
Zdeněk Doležel, Dana Novotná, Helena Schneiderová, Jan Papež, Martin Jouza
Pediatrie pro praxi.2016; 17(6): 379. CrossRef
- Thyroid
- Lack of Associations between Body Mass Index and Clinical Outcomes in Patients with Papillary Thyroid Carcinoma
-
Hyemi Kwon, Mijin Kim, Yun Mi Choi, Eun Kyung Jang, Min Ji Jeon, Won Gu Kim, Tae Yong Kim, Young Kee Shong, Dong Eun Song, Jung Hwan Baek, Suck Joon Hong, Won Bae Kim
-
Endocrinol Metab. 2015;30(3):305-311. Published online November 26, 2014
-
DOI: https://doi.org/10.3803/EnM.2015.30.3.305
-
-
4,208
View
-
39
Download
-
13
Web of Science
-
14
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Obesity is associated with aggressive pathological features and poor clinical outcomes in breast and prostate cancers. In papillary thyroid carcinoma (PTC), these relationships remain still controversial. This study aimed to evaluate the associations between body mass index (BMI) and the clinical outcomes of patients with PTC. MethodsThis retrospective study included 1,189 patients who underwent total thyroidectomy for PTCs equal to or larger than 1 cm in size. Clinical outcomes were evaluated and compared based on the BMI quartiles. ResultsThere were no significant associations between BMI quartiles and primary tumor size, extrathyroidal invasion, cervical lymph node metastasis, or distant metastasis. However, an increase in mean age was associated with an increased BMI (P for trend <0.001). Multifocality and advanced tumor-node-metastasis (TNM) stage (stage III or IV) were significantly associated with increases of BMI (P for trend 0.02 and <0.001, respectively). However, these associations of multifocality and advanced TNM stage with BMI were not significant in multivariate analyses adjusted for age and gender. Moreover, there were no differences in recurrence-free survivals according to BMI quartiles (P=0.26). ConclusionIn the present study, BMI was not associated with the aggressive clinicopathological features or recurrence-free survivals in patients with PTC.
-
Citations
Citations to this article as recorded by  - A Data-Driven Approach to Refine Predictions of Differentiated Thyroid Cancer Outcomes: A Prospective Multicenter Study
Giorgio Grani, Michele Gentili, Federico Siciliano, Domenico Albano, Valentina Zilioli, Silvia Morelli, Efisio Puxeddu, Maria Chiara Zatelli, Irene Gagliardi, Alessandro Piovesan, Alice Nervo, Umberto Crocetti, Michela Massa, Maria Teresa Samà, Chiara Mel
The Journal of Clinical Endocrinology & Metabolism.2023; 108(8): 1921. CrossRef - Potential impact of obesity on the aggressiveness of low- to intermediate-risk papillary thyroid carcinoma: results from a MASTER cohort study
Mijin Kim, Yae Eun Kang, Young Joo Park, Bon Seok Koo, Eu Jeong Ku, June Young Choi, Eun Kyung Lee, Bo Hyun Kim
Endocrine.2023; 82(1): 134. CrossRef - Potential Impact of Body Mass Index on the Clinical Outcome of Papillary Thyroid Cancer After High-Dose Radioactive Iodine Therapy
Jingjia Cao, Xiaolu Zhu, Yaru Sun, Xiao Li, Canhua Yun, Wei Zhang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Nutritional status and follicular-derived thyroid cancer: An update
Luigi Barrea, Marco Gallo, Rosaria Maddalena Ruggeri, Paola Di Giacinto, Franz Sesti, Natalie Prinzi, Valerio Adinolfi, Viola Barucca, Valerio Renzelli, Giovanna Muscogiuri, Annamaria Colao, Roberto Baldelli
Critical Reviews in Food Science and Nutrition.2021; 61(1): 25. CrossRef - Effects of concomitant obesity and diabetes on the aggressiveness and outcomes of differentiated thyroid cancer patients
Onur Elbasan, Dilek Gogas Yavuz
Archives of Endocrinology and Metabolism.2021;[Epub] CrossRef - Association of BMI with Clinicopathological Features of Papillary Thyroid Cancer: A Systematic Review and Meta‐Analysis
R. J. O'Neill, S. Abd Elwahab, M. J. Kerin, A. J. Lowery
World Journal of Surgery.2021; 45(9): 2805. CrossRef - Association Between Aggressive Clinicopathologic Features of Papillary Thyroid Carcinoma and Body Mass Index: A Systematic Review and Meta-Analysis
Aliki Economides, Konstantinos Giannakou, Ioannis Mamais, Panayiotis A. Economides, Panagiotis Papageorgis
Frontiers in Endocrinology.2021;[Epub] CrossRef - Potential Impact of BMI on the Aggressiveness of Presentation and Clinical Outcome of Differentiated Thyroid Cancer
Antonio Matrone, Giovanni Ceccarini, Marianna Beghini, Federica Ferrari, Carla Gambale, Mariaida D’Aqui, Paolo Piaggi, Liborio Torregrossa, Eleonora Molinaro, Fulvio Basolo, Paolo Vitti, Ferruccio Santini, Rossella Elisei
The Journal of Clinical Endocrinology & Metabolism.2020; 105(4): e1124. CrossRef - Correlation between obesity and clinicopathological characteristics in patients with papillary thyroid cancer: a study of 1579 cases: a retrospective study
Huijuan Wang, Pingping Wang, Yu Wu, Xiukun Hou, Zechun Peng, Weiwei Yang, Lizhao Guan, Linfei Hu, Jingtai Zhi, Ming Gao, Xiangqian Zheng
PeerJ.2020; 8: e9675. CrossRef - Lack of association between obesity and aggressiveness of differentiated thyroid cancer
G. Grani, L. Lamartina, T. Montesano, G. Ronga, V. Maggisano, R. Falcone, V. Ramundo, L. Giacomelli, C. Durante, D. Russo, M. Maranghi
Journal of Endocrinological Investigation.2019; 42(1): 85. CrossRef - Mitochondrial DNA haplogroup K as a contributor to protection against thyroid cancer in a population from southeast Europe
Relu Cocoş, Sorina Schipor, Corin Badiu, Florina Raicu
Mitochondrion.2018; 39: 43. CrossRef - The impact of BMI on clinical progress, response to treatment, and disease course in patients with differentiated thyroid cancer
Danuta Gąsior-Perczak, Iwona Pałyga, Monika Szymonek, Artur Kowalik, Agnieszka Walczyk, Janusz Kopczyński, Katarzyna Lizis-Kolus, Tomasz Trybek, Estera Mikina, Dorota Szyska-Skrobot, Klaudia Gadawska-Juszczyk, Stefan Hurej, Artur Szczodry, Anna Słuszniak,
PLOS ONE.2018; 13(10): e0204668. CrossRef - Pretreatment BMI Is Associated with Aggressive Clinicopathological Features of Papillary Thyroid Carcinoma: A Multicenter Study
Shi-tong Yu, Wanzhi Chen, Qian Cai, Faya Liang, Debin Xu, Ping Han, Jichun Yu, Xiaoming Huang
International Journal of Endocrinology.2017; 2017: 1. CrossRef - Associations between body mass index and lymph node metastases of patients with papillary thyroid cancer
Changhua Wu, Liang Wang, Wanjun Chen, Shujuan Zou, Aiju Yang
Medicine.2017; 96(9): e6202. CrossRef
- Thyroid
- Erratum: Figure Correction: Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010
-
Yun Mi Choi, Tae Yong Kim, Eun Kyung Jang, Hyemi Kwon, Min Ji Jeon, Won Gu Kim, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2015;30(1):116. Published online March 27, 2015
-
DOI: https://doi.org/10.3803/EnM.2015.30.1.116
-
-
 PDF PDF PubReader PubReader
- Thyroid
- Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010
-
Yun Mi Choi, Tae Yong Kim, Eun Kyung Jang, Hyemi Kwon, Min Ji Jeon, Won Gu Kim, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2014;29(4):530-535. Published online December 29, 2014
-
DOI: https://doi.org/10.3803/EnM.2014.29.4.530
-
-
4,235
View
-
39
Download
-
23
Web of Science
-
36
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
The prevalence of thyroid cancer has increased very rapidly in Korea. However, there is no published report focusing on thyroid cancer mortality in Korea. In this study, we aimed to evaluate standardized thyroid cancer mortality using data from Statistics Korea (the Statistical Office of Korea). MethodsPopulation and mortality data from 1985 to 2010 were obtained from Statistics Korea. Age-standardized rates of thyroid cancer mortality were calculated according to the standard population of Korea, as well as World Health Organization (WHO) standard population and International Cancer Survival Standard (ICSS) population weights. ResultsThe crude thyroid cancer mortality rate increased from 0.1 to 0.7 per 100,000 between 1985 and 2010. The pattern was the same for both sexes. The age-standardized mortality rate (ASMR) for thyroid cancer for Korean resident registration population increased from 0.19 to 0.67 between 1985 and 2000. However, it decreased slightly, from 0.67 to 0.55, between 2000 and 2010. When mortality was adjusted using the WHO standard population and ICSS population weights, the ASMR similarly increased until 2000, and then decreased between 2000 and 2010. ConclusionThyroid cancer mortality increased until 2000 in Korea. It started to decrease from 2000.
-
Citations
Citations to this article as recorded by  - Trends in incidence and overdiagnosis of thyroid cancer in China, Japan, and South Korea
Yongtian Lin, Yu Wu
Cancer Science.2023; 114(10): 4052. CrossRef - Risk of Adverse Pregnancy Outcomes in Young Women with Thyroid Cancer: A Systematic Review and Meta-Analysis
Shinje Moon, Ka Hee Yi, Young Joo Park
Cancers.2022; 14(10): 2382. CrossRef - Asymptomatic Patients and Rising Incidence of Thyroid Cancer—Reply
Mirabelle Sajisevi, Louise Davies
JAMA Otolaryngology–Head & Neck Surgery.2022; 148(12): 1186. CrossRef - Asymptomatic Patients and Rising Incidence of Thyroid Cancer
Shijie Yang, Xiequn Xu
JAMA Otolaryngology–Head & Neck Surgery.2022; 148(12): 1185. CrossRef - Does the radioactive iodine dose affect smell, taste sensation and nose function?
B Tutar, T Özülker, G Berkiten, S Karaketir, M E Ekincioğlu, Z Saltürk, Ö Onaran, B Gürpınar, Ş Karaketir, T L Kumral, Y Uyar
The Journal of Laryngology & Otology.2021; 135(1): 50. CrossRef - Disparities in Cancer-Related Avoidable Mortality by the Level of Area Deprivation in South Korea
Woorim Kim, Seongkyeong Jang, Gangeun Lee, Yoon Jung Chang
International Journal of Environmental Research and Public Health.2021; 18(15): 7856. CrossRef - Thyroid cancer: incidence and mortality trends in China, 2005–2015
Junyi Wang, Fangfang Yu, Yanna Shang, Zhiguang Ping, Li Liu
Endocrine.2020; 68(1): 163. CrossRef - A miRNA-clinicopathological nomogram for the prediction of central lymph node metastasis in papillary thyroid carcinoma-analysis from TCGA database
Mingjun Wang, Rongjing Li, Xiuhe Zou, Tao Wei, Rixiang Gong, Jingqiang Zhu, Zhihui Li
Medicine.2020; 99(35): e21996. CrossRef - Trends in the Diagnosis and Treatment of Patients with Medullary Thyroid Carcinoma in Korea
Hwa Young Ahn, Jae Eun Chae, Hyemi Moon, Junghyun Noh, Young Joo Park, Sin Gon Kim
Endocrinology and Metabolism.2020; 35(4): 811. CrossRef - Optimal Thyrotropin Suppression Therapy in Low-Risk Thyroid Cancer Patients after Lobectomy
Lee, Jeon, Kim, Sung, Chung, Shong, Hong
Journal of Clinical Medicine.2019; 8(9): 1279. CrossRef - Improved survival after early detection of asymptomatic distant metastasis in patients with thyroid cancer
Hosu Kim, So Young Park, Jaehoon Jung, Jung-Han Kim, Soo Yeon Hahn, Jung Hee Shin, Young Lyun Oh, Man Ki Chung, Hye In Kim, Sun Wook Kim, Jae Hoon Chung, Tae Hyuk Kim
Scientific Reports.2019;[Epub] CrossRef - Do aggressive variants of papillary thyroid carcinoma have worse clinical outcome than classic papillary thyroid carcinoma?
Eyun Song, Min Ji Jeon, Hye-Seon Oh, Minkyu Han, Yu-Mi Lee, Tae Yong Kim, Ki-Wook Chung, Won Bae Kim, Young Kee Shong, Dong Eun Song, Won Gu Kim
European Journal of Endocrinology.2018; 179(3): 135. CrossRef - Study Protocol of Multicenter Prospective Cohort Study of Active Surveillance on Papillary Thyroid Microcarcinoma (MAeSTro)
Jae Hoon Moon, Ji-hoon Kim, Eun Kyung Lee, Kyu Eun Lee, Sung Hye Kong, Yeo Koon Kim, Woo-jin Jung, Chang Yoon Lee, Roh-Eul Yoo, Yul Hwangbo, Young Shin Song, Min Joo Kim, Sun Wook Cho, Su-jin Kim, Eun Jae Jung, June Young Choi, Chang Hwan Ryu, You Jin Lee
Endocrinology and Metabolism.2018; 33(2): 278. CrossRef - Surgeon volume and prognosis of patients with advanced papillary thyroid cancer and lateral nodal metastasis
H I Kim, T H Kim, J-H Choe, J-H Kim, J S Kim, Y N Kim, H Kim, S W Kim, J H Chung
British Journal of Surgery.2018; 105(3): 270. CrossRef - Ultrasound requested by general practitioners or for symptoms unrelated to the thyroid gland may explain higher prevalence of thyroid nodules in females
Ana Germano, Willian Schmitt, Pedro Almeida, Rui Mateus-Marques, Valeriano Leite
Clinical Imaging.2018; 50: 289. CrossRef - Associations between Hashimoto Thyroiditis and Clinical Outcomes of Papillary Thyroid Cancer: A Meta-Analysis of Observational Studies
Shinje Moon, Hye Soo Chung, Jae Myung Yu, Hyung Joon Yoo, Jung Hwan Park, Dong Sun Kim, Young Joo Park
Endocrinology and Metabolism.2018; 33(4): 473. CrossRef - Refining the eighth edition AJCC TNM classification and prognostic groups for papillary thyroid cancer with lateral nodal metastasis
Hye In Kim, Kyunga Kim, So Young Park, Jun-Ho Choe, Jung-Han Kim, Jee Soo Kim, Young Lyun Oh, Soo Yeon Hahn, Jung Hee Shin, Hyeon Seon Ahn, Sun Wook Kim, Tae Hyuk Kim, Jae Hoon Chung
Oral Oncology.2018; 78: 80. CrossRef - Decreasing Disease-Specific Mortality of Differentiated Thyroid Cancer in Korea: A Multicenter Cohort Study
Min Ji Jeon, Hee Kyung Kim, Eun Heui Kim, Eun Sook Kim, Hyon-Seung Yi, Tae Yong Kim, Ho-Cheol Kang, Young Kee Shong, Won Bae Kim, Bo Hyun Kim, Won Gu Kim
Thyroid.2018; 28(9): 1121. CrossRef - Are pregnancy, parity, menstruation and breastfeeding risk factors for thyroid cancer? Results from the Korea National Health and Nutrition Examination Survey, 2010‐2015
Hosu Kim, Kyong Young Kim, Jong Ha Baek, Jaehoon Jung
Clinical Endocrinology.2018; 89(2): 233. CrossRef - Case–Control Study of Papillary Thyroid Carcinoma on Urinary and Dietary Iodine Status in South Korea
Joon‐Hyop Lee, Ra‐Yeong Song, Jin Wook Yi, Hyeong Won Yu, Hyungju Kwon, Su‐jin Kim, Young Jun Chai, June Young Choi, Jae Hoon Moon, Kyu Eun Lee, Young Joo Park, Sue K. Park
World Journal of Surgery.2018; 42(5): 1424. CrossRef - Patterns of Initial Recurrence in Completely Resected Papillary Thyroid Carcinoma
Hosu Kim, Tae Hyuk Kim, Jun-Ho Choe, Jung-Han Kim, Jee Soo Kim, Young Lyun Oh, Soo Yeon Hahn, Jung Hee Shin, Sang ah Chi, Sin-Ho Jung, Young Nam Kim, Hye In Kim, Sun Wook Kim, Jae Hoon Chung
Thyroid.2017; 27(7): 908. CrossRef - Changes in standardized mortality rates from thyroid cancer in Korea between 1985 and 2015: Analysis of Korean national data
Yun Mi Choi, Won Gu Kim, Hyemi Kwon, Min Ji Jeon, Minkyu Han, Tae Yong Kim, Young Kee Shong, Sang Mo Hong, Eun‐Gyoung Hong, Won Bae Kim
Cancer.2017; 123(24): 4808. CrossRef - Thyrotropin Suppressive Therapy for Low-Risk Small Thyroid Cancer: A Propensity Score–Matched Cohort Study
Suyeon Park, Won Gu Kim, Minkyu Han, Min Ji Jeon, Hyemi Kwon, Mijin Kim, Tae-Yon Sung, Tae Yong Kim, Won Bae Kim, Suck Joon Hong, Young Kee Shong
Thyroid.2017; 27(9): 1164. CrossRef - Preoperative serum thyroglobulin predicts initial distant metastasis in patients with differentiated thyroid cancer
Hosu Kim, Young Nam Kim, Hye In Kim, So Young Park, Jun-Ho Choe, Jung-Han Kim, Jee Soo Kim, Jae Hoon Chung, Tae Hyuk Kim, Sun Wook Kim
Scientific Reports.2017;[Epub] CrossRef - Young Age and Male Sex Are Predictors of Large-Volume Central Neck Lymph Node Metastasis in Clinical N0 Papillary Thyroid Microcarcinomas
Hye-Seon Oh, Suyeon Park, Mijin Kim, Hyemi Kwon, Eyun Song, Tae-Yon Sung, Yu-Mi Lee, Won Gu Kim, Tae Yong Kim, Young Kee Shong, Won Bae Kim, Min Ji Jeon
Thyroid.2017; 27(10): 1285. CrossRef - Restratification of survival prognosis of N1b papillary thyroid cancer by lateral lymph node ratio and largest lymph node size
Hye In Kim, Tae Hyuk Kim, Jun‐Ho Choe, Jung‐Han Kim, Jee Soo Kim, Young Lyun Oh, Soo Yeon Hahn, Jung Hee Shin, Hye Won Jang, Young Nam Kim, Hosu Kim, Hyeon Seon Ahn, Kyunga Kim, Sun Wook Kim, Jae Hoon Chung
Cancer Medicine.2017; 6(10): 2244. CrossRef - Risk factors associated with high thyroglobulin level following radioactive iodine ablation, measured 12 months after treatment for papillary thyroid carcinoma
Eun Young Kim, Kee Hoon Hyun, Yong Lai Park, Chan Heun Park, Ji-Sup Yun
Annals of Surgical Treatment and Research.2017; 92(1): 1. CrossRef - Disease-Specific Mortality of Differentiated Thyroid Cancer Patients in Korea: A Multicenter Cohort Study
Min Ji Jeon, Won Gu Kim, Tae Hyuk Kim, Hee Kyung Kim, Bo Hyun Kim, Hyon-Seung Yi, Eun Sook Kim, Hosu Kim, Young Nam Kim, Eun Heui Kim, Tae Yong Kim, Sun Wook Kim, Ho-Cheol Kang, Jae Hoon Chung, Young Kee Shong, Won Bae Kim
Endocrinology and Metabolism.2017; 32(4): 434. CrossRef - Features of papillary thyroid microcarcinoma associated with lateral cervical lymph node metastasis
Min Ji Jeon, Mi Sun Chung, Hyemi Kwon, Mijin Kim, Suyeon Park, Jung Hwan Baek, Dong Eun Song, Tae‐Yon Sung, Suck Joon Hong, Tae Yong Kim, Won Bae Kim, Young Kee Shong, Jeong Hyun Lee, Won Gu Kim
Clinical Endocrinology.2017; 86(6): 845. CrossRef - Dynamic Risk Stratification for Predicting Recurrence in Patients with Differentiated Thyroid Cancer Treated Without Radioactive Iodine Remnant Ablation Therapy
Suyeon Park, Won Gu Kim, Eyun Song, Hye-Seon Oh, Mijin Kim, Hyemi Kwon, Min Ji Jeon, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Thyroid.2017; 27(4): 524. CrossRef - Clinical outcomes of low-dose and high-dose postoperative radioiodine therapy in patients with intermediate-risk differentiated thyroid cancer
Ju Hye Jeong, Eun Jung Kong, Shin Young Jeong, Sang-Woo Lee, Ihn Ho Cho, Kyung Ah Chun, Jaetae Lee, Byeong-Cheol Ahn
Nuclear Medicine Communications.2017; 38(3): 228. CrossRef - Single-Incision, Gasless, Endoscopic Trans-Axillary Total Thyroidectomy: A Feasible and Oncologic Safe Surgery in Patients with Papillary Thyroid Carcinoma
Eun Young Kim, Kwan Ho Lee, Yong Lai Park, Chan Heun Park, Cho Rok Lee, Jong Ju Jeong, Kee-Hyun Nam, Woong Youn Chung, Ji-Sup Yun
Journal of Laparoendoscopic & Advanced Surgical Techniques.2017; 27(11): 1158. CrossRef - Prognostic value of the eighth edition AJCC TNM classification for differentiated thyroid carcinoma
Tae Hyuk Kim, Young Nam Kim, Hye In Kim, So Young Park, Jun-Ho Choe, Jung-Han Kim, Jee Soo Kim, Young Lyun Oh, Soo Yeon Hahn, Jung Hee Shin, Kyunga Kim, Jong Gill Jeong, Sun Wook Kim, Jae Hoon Chung
Oral Oncology.2017; 71: 81. CrossRef - Changing trends in the clinicopathological features and clinical outcomes of medullary thyroid carcinoma
Hyemi Kwon, Won Gu Kim, Tae‐Yon Sung, Min Ji Jeon, Dong Eun Song, Yu‐Mi Lee, Jong Ho Yoon, Ki‐Wook Chung, Suck Joon Hong, Jung Hwan Baek, Jeong Hyun Lee, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Journal of Surgical Oncology.2016; 113(2): 152. CrossRef - Thyroid lobectomy with minimal incision approach
Tsuyoshi Kojima, Kazuhiko Shoji, Ryusuke Hori, Yusuke Okanoue, Shintaro Fujimura, Hideaki Okuyama, Masayuki Kitano
JOURNAL OF JAPAN SOCIETY FOR HEAD AND NECK SURGERY.2016; 26(2): 283. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef
- Thyroid
- Solitary Skin Metastasis of Papillary Thyroid Carcinoma
-
Hyemi Kwon, Hyojung Kim, Sojung Park, Dong Eun Song, Won Gu Kim, Tae Yong Kim, Young Kee Shong, Won Bae Kim
-
Endocrinol Metab. 2014;29(4):579-583. Published online December 29, 2014
-
DOI: https://doi.org/10.3803/EnM.2014.29.4.579
-
-
4,014
View
-
41
Download
-
7
Web of Science
-
8
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
A solitary skin metastasis is a rare manifestation of papillary thyroid carcinoma (PTC). A 55-year-old woman presented with a movable subcutaneous nodule in her anterior neck for several months. Three years ago, she underwent total thyroidectomy and remnant ablation for classical PTC (pT3N0M0) and was under thyroxine suppression therapy without any evidence of recurrent disease. The subcutaneous nodule was 0.4 cm in size, firm, and movable without any change in the overlying skin. Recurrent PTC was confirmed after excision biopsy. Eight months after, she got a new nodule along the previous excision site. After punch biopsy, metastatic PTC was confirmed in the deep dermis and was re-excised with a clear resection margin. This is the first report of a case of solitary skin metastasis of PTC in Korea. Although solitary skin metastasis of PTC is rare, it should be considered in patients with a skin nodule. -
Citations
Citations to this article as recorded by  - Skin Metastasis Occurring 30 Years After Thyroidectomy for Papillary Thyroid Carcinoma
Mohammed S Alwhaid, Olaa Mhish, Mutahir A Tunio, Salman AlMalki, Mushabbab Al Asiri, Khalid Al-Qahtani
Cureus.2022;[Epub] CrossRef - Solitary Nasopharyngeal Metastasis From Papillary Thyroid Carcinoma Shown on FDG PET/CT
Anqi Xu, Xiao Jie, Yan Xiu, Hongcheng Shi
Clinical Nuclear Medicine.2022; 47(5): e425. CrossRef - PD-L1-positive Anaplastic Transformation in a BRAF V600E Expressing Papillary Thyroid Carcinoma with Cutaneous Metastasis: An Unusual Case Report
Pooja Ramakant, Anand Mishra, Chanchal Rana, Kulranjan Singh
Indian Journal of Endocrine Surgery and Research.2022; 17(1): 21. CrossRef - Unusual Thyroid Carcinoma Metastases: a Case Series and Literature Review
Eleonora Farina, Fabio Monari, Giovanni Tallini, Andrea Repaci, Renzo Mazzarotto, Francesca Giunchi, Riccardo Panzacchi, Silvia Cammelli, Gilbert D. A. Padula, Francesco Deodato, Renato Pasquali, Stefano Fanti, Michelangelo Fiorentino, Alessio G. Morganti
Endocrine Pathology.2016; 27(1): 55. CrossRef - Skin manifestations of endocrine and neuroendocrine tumors
Jonathan S. Leventhal, Irwin M. Braverman
Seminars in Oncology.2016; 43(3): 335. CrossRef - Isolated Metastasis in Male Breast from Differentiated Thyroid Carcinoma – Oncological Curiosity. A Case Report and Review of Literature
Lakshminarasimman Parasuraman, Shubhada V. Kane, Prathamesh S. Pai, Kintan Shanghvi
Indian Journal of Surgical Oncology.2016; 7(1): 91. CrossRef - A Closer Look at Papillary Thyroid Carcinoma
Won Bae Kim
Endocrinology and Metabolism.2015; 30(1): 1. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef
|